Circulating tumor cells can reveal genetic signature of dangerous lung cancers
Massachusetts General Hospital (MGH) investigators have shown that an MGH-developed, microchip-based device that detects and analyzes tumor cells in the bloodstream can be used to determine the genetic signature of lung tumors, allowing identification of those appropriate for targeted treatment and monitoring genetic changes that occur during therapy. A pilot study of the device called the CTC-chip will appear in the July 24 New England Journal of Medicine and is receiving early online release.
"The CTC-chip opens up a whole new field of studying tumors in real time," says Daniel Haber, MD, director of the MGH Cancer Center and the study's senior author. "When the device is ready for larger clinical trials, it should give us new options for measuring treatment response, defining prognostic and predictive measures, and studying the biology of blood-borne metastasis, which is the primary method by which cancer spreads and becomes lethal."
CTCs or circulating tumor cells are living solid-tumor cells found at extremely low levels in the bloodstream. Until the development of the CTC-chip by researchers from the MGH Cancer Center and BioMEMS (BioMicroElectroMechanical Systems) Resource Center, it was not possible to get information from CTCs that would be useful for clinical decision-making. The current study was designed to find whether the device could go beyond detecting CTCs to helping analyze the genetic mutations that can make a tumor sensitive to treatment with targeted therapy drugs.
The researchers tested blood samples from patients with non-small-cell lung cancer (NSCLC), the leading cause of cancer death in the U.S. In 2004, MGH researchers and a team from Dana-Farber Cancer Institute both discovered that mutations in a protein called EGFR determine whether NSCLC tumors respond to a group of drugs called TKIs, which includes Iressa and Tarceva. Although the response of sensitive tumors to those drugs can be swift and dramatic, eventually many tumors become resistant to the drugs and resume growing.
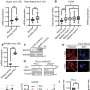
The CTC-chip was used to analyze blood samples from 27 patients – 23 who had EGFR mutations and 4 who did not – and CTCs were identified in samples from all patients. Genetic analysis of CTCs from mutation-positive tumors detected those mutations 92 percent of the time. In addition to the primary mutation that leads to initial tumor development and TKI sensitivity, the CTC-chip also detected a secondary mutation associated with treatment resistance in some participants, including those whose tumors originally responded to treatment but later resumed growing.
"Patients found to have resistance mutations before treatment probably won't benefit as much or as long from single-agent TKI therapy as those without such baseline mutations," says Lecia Sequist, MD, MPH, of the MGH Cancer Center, a co-lead author of the NEJM paper. "For those patients we may need to consider other modes of therapy, including combinations+ of targeting agents or second-generation TKIs that can overcome the most common resistance mutation."
Blood samples were taken at regular intervals during the course of treatment from four patients with mutation-positive tumors. In all of those patients, levels of CTCs dropped sharply after TKI treatment began and began rising when tumors resumed growing. In one patient, adding additional chemotherapy caused CTC levels to drop again as the tumor continued shrinking.
Throughout the course of therapy, the tumors' genetic makeup continued to evolve. Not only did the most common resistance mutation emerge in tumors where it was not initially present, but new activating mutations – the type that causes a tumor to develop in the first place – appeared in seven patients' tumors, indicating that these cancers are more genetically complex than expected and that continuing to monitor tumor genotype throughout the course of treatment may be crucial.
"If tumor genotypes don't remain static during therapy, it's essential to know exactly what you're treating at the time you are treating it," says Haber. "Biopsy samples taken at the time of diagnosis can never tell us about changes emerging during therapy or genotypic differences that may occur in different sites of the original tumor, but the CTC-chip offers the promise of noninvasive continuous monitoring." Haber is the Kurt J. Isselbacher/Peter D. Schwartz Professor of Medicine at Harvard Medical School.
Source: Massachusetts General Hospital