'Smart scaffolds' may help heal broken hearts
Canadian researchers have, for the first time, developed an organic substance that attracts and supports cells necessary for tissue repair and can be directly injected into problem areas. This development, published online in the FASEB Journal, is a major step toward treatments that allow people to more fully recover from injury and disease and may even help reduce the need for organ transplantation.
Imagine new treatments for heart disease or muscle loss that direct the body to repair damaged tissue rather than helping it cope with a weakened condition. That's not hard to do thanks to Canadian researchers, who for the first time, have developed an organic substance that attracts and supports cells necessary for tissue repair and can be directly injected into problem areas. This development, published online in The FASEB Journal is a major step toward treatments that allow people to more fully recover from injury and disease rather than having to live with chronic health problems. It may even help reduce the need for organ transplantation by allowing physicians to save organs that would have been previously damaged beyond repair.
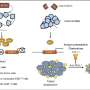
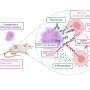
The "smart scaffolds," developed by Erik Suuronen and his colleagues from the University of Ottawa and the Ottawa Heart Research Institute, work because they contain a protein that allows progenitor cells to adhere to the damaged tissue and survive long enough to promote healing. These cells emit homing signals that summon other cells to join in the process and give off chemical signals that order cells to grow blood vessels necessary for healing to occur.
"Ultimately, we envision a scaffold material that can be taken off the shelf and injected into the hearts of patients suffering from blocked arteries," said Suuronen. "The scaffold materials would direct the repair process, and restore blood flow and function to the heart."
The researchers tested this material in three groups of rats, with each group suffering from a lack of blood oxygen (ischemia) to their thigh muscles. The muscles in the first group of rats were treated with the smart scaffold. The second group of rats received a scaffold not engineered for cell attachment. The third group received a placebo. Two weeks after treatment, rats treated with the "smart" scaffold had more new blood vessels and better functional recovery while rats from the other two groups of rats only had minimal improvement.
"This is a major development toward radically new treatments for heart and muscle disease," said Gerald Weissmann, M.D., Editor-in-Chief of The FASEB Journal. "If this research holds up in humans, it has the potential to save more lives than any other major advance in the field since the stent."
Article Details: Erik J. Suuronen, Pingchuan Zhang, Drew Kuraitis, Xudong Cao, Angela Melhuish, Daniel McKee, Fengfu Li, Thierry G. Mesana, John P. Veinot, and Marc Ruel. An acellular matrix-bound ligand enhances the mobilization, recruitment and therapeutic effects of circulating progenitor cells in a hindlimb ischemia model.doi:10.1096/fj.08-111054. www.fasebj.org/cgi/content/abstract/fj.08-111054v1
Source: Federation of American Societies for Experimental Biology