Scientists reveal a new mechanism that increases atherosclerosis in mice
(PhysOrg.com) -- For all the good it does, a liver protein that senses and gets rid of drugs and pollutants from our body has a downside. For the first time, it has been shown that when it is chronically activated, the protein, called PXR, rejiggers how cholesterol is processed in the liver and increases the risk of developing atherosclerosis. The work has direct clinical consequences to patients under long-term treatment of PXR-activating drugs, including several antibiotic and anti-cancer medications — and your daily latte.
A shot of espresso may rev you up in the morning, but the downside is that it may also ramp up levels of bad cholesterol due to its effects on a unique liver protein called PXR. New research from Rockefeller University now shows that when chronically activated, the protein rejiggers how cholesterol is broken down in and cleared from the liver, a disturbance that can lead to high levels of the waxy substance or worse, full-blown atherosclerosis.
“It’s the first time that PXR has been shown to have a direct impact on balancing cholesterol levels in the body,” says first author Changcheng Zhou, a research associate in Jan L. Breslow’s Laboratory of Biochemical Genetics and Metabolism at Rockefeller.
Unlike other receptor proteins, which can recognize only one or a few chemicals, PXR — short for pregnane x receptor — can recognize more than a hundred, including cafestrol, present in unfiltered brewed coffee, and many prescription medications. The research, led by Breslow, may have direct clinical consequences for patients taking drugs such as the antibiotic rifampicin for tuberculosis treatment, the antiretroviral drug ritonavir for HIV treatment and the antiepileptic drugs carbamazipine and phenobarbital, all of which activate PXR.
“At the time these drugs were being developed — the antivirals, the antibiotics, anti-cancers and even herbal supplements like St. John’s Wort — their interactions with PXR weren’t known,” explains Zhou. “Now patients under long-term treatment with PXR-activating drugs can be more informed about these drugs’ effects.”
When activated, PXR, which resides in the nucleus of liver cells in all animals, including humans, latches on to strips of DNA and turns on genes that regulate how chemicals or drugs are metabolized and cleared from the liver. Many drugs that can activate PXR have been shown to increase cholesterol levels in patients, and too much of the stuff in the bloodstream is a well-established risk factor for cardiovascular disease, the nation’s biggest killer. However, it was not clear whether PXR could jumpstart this process.
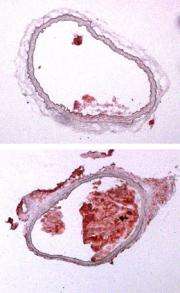
In their work, Zhou and Breslow introduced a mouse-specific PXR activator called PCN into the diets of normal mice for two weeks and found that while their levels of good cholesterol, or HDL, were not affected, their levels of bad cholesterol skyrocketed six-fold. Another group of mice that were fed PCN for eight weeks and were genetically engineered to lack the protein ApoE experienced the flipside: Their good cholesterol plummeted and they also went on to develop full-blown atherosclerosis.
Several gene targets of PXR were the same for both normal mice and those lacking the ApoE protein, including a cholesterol metabolism enzyme called CYP39A1 and a transportation protein called Apo-IV. A gene called CD36 was another target specifically associated with the uptake of modified bad cholesterol by certain cells, which contribute to the accumulation of artery-clogging fat.
To Zhou, this research is only the beginning. “Many chemicals exposed in the air are also PXR activators,” says Zhou. “So what we have in our hands now may not only be a heart health issue but also a public health one.”
More information: Journal of Lipid Research 50(10): 2004-2013 (October 1, 2009) Activation of PXR induces hypercholesterolemia in wild-type and accelerates atherosclerosis in apoE deficient mice, Changcheng Zhou, Nakesha King, Kwan Y. Chen and Jan L. Breslow
Provided by Rockefeller University (news : web)















