New structure of an important immune system complex resolves a 10-year controversy
(Medical Xpress) -- Researchers at the University of Toronto and the University of Bath have resolved a longstanding controversy surrounding an important structure of the immune system that could result in new therapeutic targets for antibody-mediated autoimmune diseases as well as the potential to enhance the efficacy of vaccines.
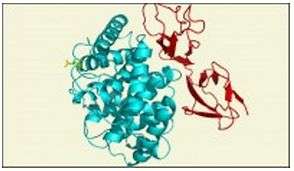
In a study published in the April 29 issue of Science, Professor David Isenman of biochemistry and Jean van den Elsen of the University of Bath shed light on the complex between complement receptor 2 and its ligand C3d, both of which are constituents of an innate immune system of our body known as complement.
“We recognize that the goal of applying this knowledge to autoimmune therapies and enhanced vaccine efficiency will not be trivial. But the structural scaffold for further discoveries is now in place,” said Isenman.
The detailed knowledge of the receptor-ligand interface provided by the new structure of this complex has implications as both a potential therapeutic target, in the case of antibody-mediated autoimmune diseases, and as something that may be exploited in enhancing the efficacy of vaccines.
The role of complement in mediating the clearance of microbial pathogens, either directly or in conjunction with antibodies, has long been recognized. A key element of the process is the “tagging” of the foreign target by a proteolytically activated fragment of complement component C3. This first C3 split product, as well as its subsequent degradation products, remains covalently attached to the foreign target where they act as ligands (i.e., bridging molecules) for complement receptors present on white blood cells. In turn, these white blood cells can engulf and destroy the tagged microbial target.
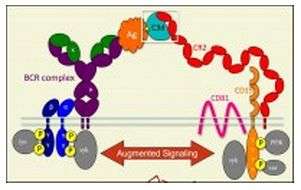
In more recent years, it has become well established that complement also plays a role in focusing the antibody arm of the adaptive immune system on an antigen which it has tagged with a C3 split product, the limit one of which is known as C3d. The latter is a ligand for complement receptor 2 (CR2) on B lymphocytes, the very type of cell that, when stimulated by a specific antigen, undergoes clonal expansion and ultimately differentiates into “factory” cells that secrete large amounts of the antibody against the antigen that was initially encountered. As illustrated in the accompanying schematic, both the antigen recognition entity of the B cell (the B cell receptor, BCR), as well as the C3d-binding CR2 molecule, are each associated with other molecules involved in generating intracellular signals that drive B cell clonal expansion. In what is known as the co-ligation model, the C3d-tagged antigen mediates a bridge between the BCR complex and the CR2/CD19/CD81 complex, the effect of which is to greatly enhance the amount of signalling relative to that achieved by antigen binding to the BCR alone. What this does is lower by orders of magnitude the threshold quantity of antigen required to initiate the antibody response of the particular B cell recognizing that particular antigen. There is an additional role for CR2 present on a different cell type, the follicular dendritic cell (FDC) of lymph nodes, in trapping C3d-tagged antigen in the lymph node. This in turn is important in generating stronger binding antibodies and in the induction of long-lived memory B cells that allows one to rapidly mount an antibody response years after the first encounter with a particular antigen. These effects, which are mediated by the CR2-C3d interactions on B cells and FDCs, are collectively referred to as the “molecular adjuvant” effects of complement and this is important in making the antibody response sensitive to the low concentrations of antigen that are present in the early stages of infection. Unfortunately, these same CR2-C3d binding events can sometimes lead to detrimental effects in the case of individuals having B cells that are reactive against self-antigens and which produce the antibodies at the root of antibody-mediated autoimmune diseases such as systemic lupus erythematosus (commonly known as lupus disease or SLE).
Clearly there is a potential to therapeutically exploit the CR2-C3d interaction, either through the rational design of drugs that would inhibit the interaction in the case of some autoimmune conditions or the rational design of small molecule CR2-binding mimetics of C3d, which may be used to decorate antigens in a subunit (i.e,. pathogen surface protein-based, as opposed to whole pathogenic microorganism-based) vaccine situation. Unfortunately, the molecular details of the CR2-C3d interface (represented within the white box of the schematic) necessary to pursue such therapeutic avenues have been mired in controversy for the past decade. Specifically, in 2001 an X-ray crystal structure of the complex consisting of C3d and the first two domains of CR2 [hereinafter denoted CR2(SCR1-2)] was published in Science, however from the start that structure was discordant with much biochemical data in the literature, and over the years the discrepancies have only increased.
“To be clear, there were no errors made in the original structure determination, but it is now apparent from extensive subsequent biochemical work that the 2001 structure represented a non-physiologic complex that resulted from the particular crystallization conditions used,” said van den Elsen.
The structure of the CR2(SCR1-2)-C3d complex from van den Elsen and Isenman was also determined using X-ray crystallography, but under more physiologic crystallization conditions. The new structure (depicted here) is very different from the previous one, but its features do conform to all existing biochemical data. With the controversy regarding atomic level details of the binding interface now finally resolved, the new structure of the CR2(SCR1-2)-C3d complex will hopefully provide the platform for both the design of compounds that may exploit this interface as either a therapeutic target or in enhancing the efficacy of vaccines. While this discovery lays an important foundation, the authors of the current study recognize that neither of these goals will be simple to achieve and will require contributions from medicinal chemists, in addition to complementologists and immunologists.

















