New technology helps fight deadly outbreaks
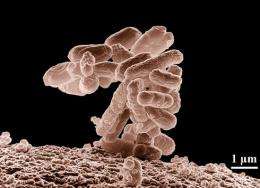
Sequencing the DNA of outbreak-causing microbes is nothing new -- but completing the entire process in a few short hours is.
The simultaneous announcement from separate research teams in Germany and China on June 2 was remarkable not only because both independent groups quickly identified the E. coli strain genome responsible for sickening thousands across Europe by using DNA sequencing machines one-tenth the size and cost of traditional sequencers, but also because of how these new machines are expected to dramatically alter how officials approach stopping outbreaks of infectious diseases.
In late May, German patients started reporting food poisoning symptoms -- intestinal cramping, fever, and bloody diarrhea -- all symptoms of E. coli infection. A few people were hospitalized with hemolytic-uremic syndrome, a rare complication that can lead to kidney failure. Public health officials had little luck determining the source of the outbreak as the number of reported cases steadily increased, so researchers began to search for answers within the disease itself by quickly sequencing a strain of E. coli believed to be the cause of the outbreak.
Both the Chinese and German teams turned to the Personal Genome Machine, a sequencing machine that arrived on the market in late 2010. The machine costs $50,000, one-tenth the cost of comparable existing machines on the market, and is roughly the size of a desktop printer.
These newest DNA sequencing machines will affect areas far beyond infectious diseases, from oncology to agriculture. But everyone is in agreement that rapid DNA sequencing will undoubtedly improve science and human health.
"Because this machine was so cheap, both groups had it," said Jonathan Rothberg, inventor of the PGM, which was recently acquired by Life Technologies. "And because they were so fast, both groups used it and literally had the sequence before they got their other machines warmed up."
Despite its speed, the PGM sequences long strands of DNA one nucleotide at a time. With one half of the DNA molecule serving as a template, the PGM uses a microchip that can sense a tiny chemical change that occurs when the machine adds a nucleotide to the growing strand of DNA. The machine gets its speed by sequencing many DNA molecules at the same time. It took scientists one year to sequence the E. coli genome in the late 90s. With the PGM, Rothberg says, researchers can do the same work in just a few hours.
DNA sequence in hand, scientists determined that the strain of E. coli implicated in the outbreak was not a new strain, as previously thought, but a hybrid of two existing strains. This knowledge will allow researchers to create rapid diagnostic tests and perhaps even identify the source of the outbreak.
"These emerging technologies are creating a revolution in public health," said Matthew Waldor, a microbiologist at Harvard University.
Although he wasn't involved with the teams that sequenced the strain for this latest outbreak, Waldor would know. Besides contributing his knowledge to solving the E. coli outbreak in Europe, Waldor and colleagues sequenced the cholera bacteria that caused an outbreak in Haiti last year. The outbreak, still ongoing, confused scientists as the cholera bacteria, Vibrio cholerae, hadn't been detected in Haiti for decades.
Waldor teamed up with Life Technologies competitor Pacific Biosciences to sequence cholera samples circulating in Haiti which were published last January in the New England Journal of Medicine. By comparing the Haiti sequences with other known cholera genomes, Waldor's team discovered that the Haiti strain had been imported from Southeast Asia. By knowing where the outbreak originated, Waldor said public health officials can take steps to prevent another importation.
Just as with the E. coli outbreak, scientists sequenced the cholera bacteria in just a few hours. Instead of detecting a chemical change as a nucleotide is added to a growing strand of DNA like the PGM, the Pacific Biosciences RS machine watches each strand of DNA grow as bases are added by DNA polymerase -- the same enzyme that your body uses to add nucleotides to DNA. The RS machine sequences so rapidly because it attaches the DNA polymerase to an aluminum chip, allowing it to more quickly add nucleotides than if the enzyme floated free in a solution, and by watching thousands of polymerases in action at the same time.
But Eric Schadt, Pacific Biosciences chief scientific officer at doesn't want to content himself with "real-time" results.
"You don't want to collect a sample, and then 10 days later find out you have SARS virus because then it's too late," said Schadt.
Instead, Schadt wants to use this latest sequencing technology to stop infectious diseases before they cause outbreaks through the creation of what he calls disease weather maps. In order to project where a virus will be tomorrow, researchers need to know where it is today, which requires rapid genetic sequencing.