Ophthalmic antibiotics associated with antimicrobial resistance after intraocular injection therapy
Repeated exposure of the eye to ophthalmic antibiotics appears to be associated with the emergence of resistant strains of microbes among patients undergoing intraocular injection therapy for neovascular retinal disease, according to a report in the September issue of Archives of Ophthalmology.
According to background information in the article, more than 8 million people in the United States are affected by age-related macular degeneration, the leading cause of blindness among individuals older than 65 years in this country. Treating the neovascular or "wet" form of the disease involves monthly injections of medication into the eye; this treatment is also being studied for eye problems related to diabetes and retina vein occlusions (obstructions of veins carrying blood from the retina). To prevent the most severe complication from intraocular injection, endophthalmitis (inflammation inside the eye), ophthalmologists routinely prescribe ophthalmic antibiotics after every injection. "Repeated exposure of ocular flora [microbes living on or inside the body], however, may select for resistant bacterial strains and cultivate 'superbugs' with multiple-drug resistance that may considerably affect the treatment of ocular infections," write the authors.
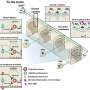
Stephen J. Kim, M.D., and Hassanain S. Toma, M.D., from the Vanderbilt University School of Medicine, Nashville, Tenn., conducted a randomized, controlled, longitudinal study of 48 eyes of 24 patients who, in one eye each, received intraocular injection. At baseline and after every injection, researchers obtained cultures of the conjunctiva (the membrane of the eye's surface and the inner eyelid) for both treated and untreated (control) eyes. Patients were randomized to one of four antibiotics and after each injection used only the antibiotic they were assigned. The researchers tested the bacterial samples for susceptibility to 16 antibiotics and analyzed the bacterial DNA. Injections were administered every four weeks for at least four consecutive months, and patients were followed for one year.
Repeated exposure to fluoroquinolone antibiotics was associated with coagulase-negative staphylococci (CNS) that demonstrated significantly increased rates of resistance to both older- and newer-generation fluoroquinolones. Repeated exposure to azithromycin was associated with CNS that demonstrated significantly increased resistance to macrolides and decreased resistance to both older- and newer-generation fluoroquinolones. Specimens of CNS from treated eyes demonstrated significant increases in multiple-drug resistance; for example, 81.8 percent of CNS specimens appeared resistant to at least three antibiotics, and 67.5 percent appeared resistant to at least five antibiotics.
The researchers suggest that their results demonstrate rapid development of resistance from CNS to certain antibiotics, and that this resistance is maintained when the antibiotic is periodically readministered. "This finding has considerable implications because conjunctival flora are presumed to be the predominant source of postinjection endophthalmitis," they write, adding that research suggests one strain of CNS is associated with greater intraocular inflammation than are strains more susceptible to antibiotics. "Our findings," the authors conclude, "indicate the need for more judicious use of ophthalmic antibiotics after intraocular injection to reduce the potential emergence and spread of antimicrobial resistance."
More information: Arch Ophthalmol. 2011;129[9]:1180-1188.