New sleep apnea device may reduce cost, time required for diagnosis
(Medical Xpress) -- UT Arlington bioengineering researchers have designed an innovative, ultrasonic sensor system that can accurately detect whether a person suffers from sleep apnea without the inconvenience or cost associated with an overnight stay in a sleep center.
The University of Texas at Arlington has applied for a provisional patent for the concept and technology. Researchers are currently identifying private partners to market the device. UT Arlington has formed an alliance with Sleep Consultants Inc. in Fort Worth to conduct studies related to the research.
Sleep apnea affects an estimated 15 percent of adults nationwide. The chronic interruption of breathing can lead to hypertension, heart failure and even some brain injuries. The new detection system promises a speedier path to diagnosis and eventual relief, said Khosrow Behbehani, professor and chair of the UT Arlington Department of Bioengineering.
“Making detection of this insidious disease more affordable will allow more people affected with the disease to be diagnosed,” Behbehani said, adding that conventional diagnostic testing can cost as much as $2,000 per patient per test. “For some, the cost is such a barrier that they may opt to continue to suffer rather than to be diagnosed.”
Ron Elsenbaumer, UT Arlington’s vice president of research and federal relations, said Behbehani’s research is representative of the kind of life-changing, biomedical research under way in the College of Engineering.
“So many people suffer from sleep apnea,” Elsenbaumer said. “That critical mass provides a built-in marketplace for the device. It’s a wonderful example of the commercially viable products that our research can provide.”
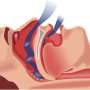
Behbehani teamed with doctoral graduate Mohammad Al-Abed and colleagues from UT Southwestern Medical Center and Sleep Consultants Inc. to develop the device, which employs ultrasonic sensors that are attached to a patient’s neck for detecting apnea during the sleep. Non-audible sound waves are sent across the neck to detect whether the patient’s airway is open to allow airflow to the lungs.
The process is less cumbersome and less expensive than current detection systems now commonly used. In most cases, a patient is asked to spend one or more nights in a sleep laboratory with a large array of electrodes and sensors attached to their body. A medical technician typically observes the patient through the night.
Behbehani said patients would be able to attach the new device themselves for overnight monitoring from the convenience of their own bed.
“In its final form, the device could be as simple as a collar wrapped around the patient’s neck,” he said.
The research advances a “smart” sleep apnea machine that Behbehani and his colleagues developed and licensed in the 1990s. That device incorporated sensors into a machine that continuously pumped air into a patient’s airway and regulated the airflow.
More than 560,000 patients have benefited from the previous invention, Behbehani said, adding that he hopes the new ultrasonic detection system will help significantly more people.
The new device was developed at the prompting of Sleep Consultants physicians who sought better care for their patients, said Dr. John Burk, medical director for Sleep Consultants and a physician with Texas Pulmonary and Critical Care Consultants. The sensors incorporated in the new, ultrasonic device can provide physicians with much more data than sleep center technicians can assemble through monitoring patients at a sleep center, he said.
“The technologies he’s developing will allow us to take a better look at our patients diagnostically,” Burk said. “In addition, it may be a very significant step in monitoring the adequacy of treatment.”