'Humanized' mice advance study of rheumatoid arthritis
Researchers at Northwestern University Feinberg School of Medicine have developed the first animal model that duplicates the human response in rheumatoid arthritis (RA), an important step that may enable scientists to discover better medicines to treat the disease.
Corresponding and senior author Harris Perlman, associate professor of rheumatology at Feinberg, introduced his team's new prototype mouse model in a recent online issue of the Journal of Translational Medicine.
"This is the first time human stem cells have been transplanted into mice in order to find RA treatments," Perlman said. "We believe this will improve drug discovery because the reactions we observed were authentic human reactions."
Until now, scientists have relied on the common scientific method of using specially bred mice to find drugs to control RA. However, human and mouse immune systems differ dramatically, so studying RA in these mice does not give an accurate representation of how the disease functions in humans. In some cases, RA drugs that seemed promising based on results in mice failed in human clinical trials.
Mice implanted with human stem cells have been used before mainly to study infectious disease.
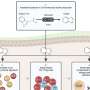
The Northwestern team injected day-old mice with human stem cells from umbilical cord blood, including white blood cells, which regulate immunity. Then, RA was introduced in the mice and suppressed with Enbrel®, a common first-line drug for joint inflammation in humans. This offered evidence that their immune systems were indeed replicating human defenses.
Scientists seek mouse models that mimic RA in humans in order to learn how the complex disease operates. In the last decade, researchers and physicians have found many subtypes of RA that originate on the molecular level and are each produced by different pathways in the body.
A debilitating disease, rheumatoid arthritis is a chronic autoimmune disorder characterized by persistent inflammation around joint areas, predominantly in the wrist and fingers. The disease causes pain, swelling, stiffness and loss of function and can result in tissue destruction. Approximately 1.3 million people have the disease.
Onset of RA usually begins between ages 25 to 55, but recent studies reveal that the disease actually begins several years before symptoms appear. This has broadened the focus to create drugs that prevent RA or at least enable early diagnosis instead of trying to reduce symptoms once it is further along and difficult to control.
This is the second mouse model Perlman has developed to help discover better rheumatoid arthritis therapies. Earlier this year, he introduced a mouse model that develops RA and is predisposed to atherosclerosis, or hardening of the arteries, a common RA complication in humans.
Perlman called this first humanized mouse model "the tip of the iceberg" in terms of how it will help improve RA treatment. He added that future studies will involve harvesting stem cells in cord blood from mothers who have RA, so researchers can work with immune cells containing the disease's genetic makeup. Since the disease is influenced by genetics, the maternal immune cells will be transplanted in mice to pinpoint preventive treatments.
Coauthors of the study at Northwestern include Alexander Misharin, research assistant professor, Shawn Rose, post-doctoral fellow, Angelica Gierut, post-doctoral fellow. Other coauthors include Kenneth Haines III, associate professor of pathology at Yale School of Medicine, and Richard Hotchkiss, professor of anesthesiology, medicine and surgery at Washington University.