Migraines associated with higher incidence of brain lesions among women; effect on health uncertain
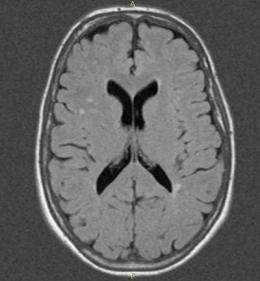
After nearly 10 years of follow-up of study participants who experienced migraines and who had brain lesions indentified via magnetic resonance imaging, women with migraines had a higher prevalence and greater increase of deep white matter hyperintensities (brain lesions) than women without migraines, although the number, frequency, and severity of migraines were not associated with lesion progression, according to a study appearing in the November 14 issue of JAMA. Also, increase in deep white matter hyperintensity volume was not significantly associated with poorer cognitive performance at follow-up.
Migraine affects up to 15 percent of the general population. "A previous cross-sectional study showed an association of migraine with a higher prevalence of magnetic resonance imaging (MRI)-measured ischemic lesions in the brain," according to background information in the article. White matter hyperintensities are associated with atherosclerotic disease risk factors, increased risk of ischemic stroke, and cognitive decline.
Inge H. Palm-Meinders, M.D., of the Leiden University Medical Center, the Netherlands, and colleagues conducted a study to determine whether women and men with migraine headaches have a higher incidence of brain lesions 9 years after initial MRI, whether migraine frequency was associated with progression of brain lesions, and whether progression of brain lesions was associated with cognitive decline. In a follow-up of the 2000 Cerebral Abnormalities in Migraine, an Epidemiological Risk Analysis cohort, which is a population-based observational study of Dutch participants with migraine and an age- and sex-matched control group, 203 of the 295 participants at the beginning of the study in the migraine group and 83 of 140 in the control group underwent MRI scan in 2009 to identify progression of MRI-measured brain lesions. Comparisons were adjusted for age, sex, hypertension, diabetes, and educational level. The participants in the migraine group were an average of 57 years of age, and 71 percent were women. Those in the control group had an average age of 55 years, and 69 percent were women.
The researchers found that of the 145 women in the migraine group, 112 (77 percent) vs. 33 of 55 women (60 percent) in the control group had progression of deep white matter hyperintensities. Among men, no association was found between migraine with progression of MRI-measured brain lesions. Although migraine was associated with a higher prevalence of infratentorial (an area of the brain) hyperintensities at follow-up, there were no significant associations of migraine with progression of infratentorial hyperintensities or posterior circulation territory infarctlike lesions among women.
"In addition, the number of migraines, frequency of migraines, migraine severity, type of migraine, and migraine therapy were not associated with lesion progression," the authors write. "Increase in deep white matter hyperintensity volume was not significantly associated with poorer cognitive performance at follow-up."
"In summary, in a community-based cohort followed up for 9 years, migraine was associated only with a higher incidence of deep white matter brain changes among women. There were no significant associations of migraine with progression of other brain lesions among women, and there were no associations of migraine headache with progression of any brain lesions among men. These findings raise questions about the role of migraine headaches with progression of cerebral vascular changes. The functional implications of MRI brain lesions in women with migraine and their possible relation with ischemia and ischemic stroke warrant further research."
In an accompanying editorial, Deborah I. Friedman, M.D., M.P.H., of the University of Texas Southwestern Medical Center, Dallas, and David W. Dodick, M.D., of the Mayo Clinic, Scottsdale, Ariz., examine the question of how the results of this study can help physicians advise patients with migraine.
"The findings imply that small white matter hyperintensities in most patients with migraine should not be a reason for alarm. However, given the relationship between migraine and several acquired and genetic vasculopathies, it is possible that certain subpopulations of patients with migraine with white matter hyperintensities may be at an increased genetic risk for significant white matter disease and neurological morbidity, including stroke, transient ischemic attack, cognitive impairment, and other neurologic outcomes. Addressing modifiable risk factors for stroke—such as obesity, smoking, hypertension, hypercholesterolemia, and physical inactivity—and avoiding high-dose combined oral contraceptives in women older than 35 years and in those with untreated or poorly controlled vascular risk factors seems prudent. Further research and advances in genetics will provide additional answers."
More information:
JAMA. 2012;308(18):1889-1897
JAMA. 2012;308(18):1920-1921













