Researchers uncover gene's role in rheumatoid arthritis, findings pave way for new treatments
University of Michigan research sheds new light on why certain people are more likely to suffer from rheumatoid arthritis – paving the way to explore new treatments for both arthritis and other autoimmune diseases.
The new UMHS research in mice identifies how a specific group of genes works behind the scenes to activate the bone-destroying cells that cause severe rheumatoid arthritis, a debilitating health issue for millions of Americans.
"We believe this could be a significant breakthrough in our understanding of why certain genes are associated with higher risk of rheumatoid arthritis and other autoimmune diseases – a link that has been a mystery in the field for decades," says lead author Joseph Holoshitz, M.D., professor of internal medicine and associate chief of research in the division of rheumatology at the U-M School of Medicine.
"We hope that this improved understanding will open the door to future design of drugs to treat this crippling disease and autoimmune disease in general."
The research appeared in The Journal of Immunology and was highlighted by Nature Reviews Rheumatology.
Rheumatoid arthritis is a chronic inflammatory disorder that damages the lining of joints and causes bone erosion, joint deformity and disability. The disease is an autoimmune disorder, characterized by the body's immune system mistakenly attacking the body's tissues.
Researchers have long studied the phenomenon of why certain versions of an inherited group of genes known as "human leukocyte antigen" (HLA) are associated with autoimmune disorders. One subset of these HLA genes that codes a protein sequence called "shared epitope" represents the most significant genetic risk factor for rheumatoid arthritis, affecting disease susceptibility and severity. However, until now, the reason for this strong link has been unclear.
A common theory in the field has been that the association between particular HLA genes and autoimmune diseases is a result of mistakenly identifying body tissues as foreign – making the body the target of the immune system and setting off an attack on self-tissues, which results in disease.
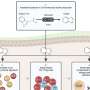
The UMHS research challenges this long-held theory. The study shows, for the first time, how this subset of HLA genes causes arthritis – by activating inflammation-causing cells, as well as bone-destroying cells (known as osteoclasts). This leads to severe arthritis and bone erosion.
"We showed how the shared epitope is directly triggering osteoclasts, the very cells that are responsible for joint destruction in people with the disease," says Holoshitz.
"Understanding these mechanisms at play could be a significant piece of future drug development. Because we now know the molecular mechanism that activates arthritis-causing cells, we have the potential to block that pathway with simple chemical compounds that could be used to treat rheumatoid arthritis and other diseases."
More information: The Journal of Immunology, Jan.3, doi:10.4049/jimmunol.1202150