Discovery opens door to new drug options for serious diseases
Researchers have discovered how oxidative stress can turn to the dark side a cellular protein that's usually benign, and make it become a powerful, unwanted accomplice in neuronal death.
This finding, reported today in Proceedings of the National Academy of Sciences, could ultimately lead to new therapeutic approaches to many of the world's debilitating or fatal diseases.
The research explains how one form of oxidative stress called tyrosine nitration can lead to cell death. Through the common link of inflammation, this may relate to health problems ranging from heart disease to chronic pain, spinal injury, cancer, aging, and amyotrophic lateral sclerosis, or Lou Gehrig's disease.
As part of the work, the scientists also identified a specific "chaperone" protein damaged by oxidants, which is getting activated in this spiral of cellular decline and death. This insight will provide a new approach to design therapeutic drugs.
The findings were published by scientists from the Linus Pauling Institute at Oregon State University; Maria Clara Franco and Alvaro Estevez, now at the University of Central Florida; and researchers from several other institutions. They culminate a decade of work.
"These are very exciting results and could begin a major shift in medicine," said Joseph Beckman.
Beckman is an LPI principal investigator, distinguished professor of biochemistry, and director of the OSU Environmental Health Sciences Center. He also last year received the Discovery Award from the Medical Research Foundation of Oregon, given to the leading medical scientist in the state.
"Preventing this process of tyrosine nitration may protect against a wide range of degenerative diseases," Beckman said. "The study shows that drugs could effectively target oxidatively-damaged proteins."
Scientists have known for decades about the general concept of oxidative damage to cells, resulting in neurodegeneration, inflammation and aging. But the latest findings prove that some molecules in a cell are thousands of times more sensitive to attack.
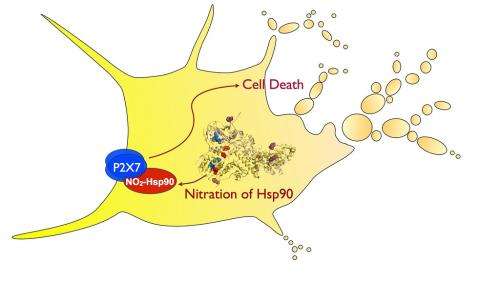
In this case, heat shock protein 90, or HSP90, helps monitor and chaperone as many as 200 necessary cell functions. But it can acquire a toxic function after nitration of a single tyrosine residue.
"It was difficult to believe that adding one nitro group to one protein will make it toxic enough to kill a motor neuron," Beckman said. "But nitration of HSP90 was shown to activate a pro-inflammatory receptor called P2X7. This begins a dangerous spiral that eventually leads to the death of motor neurons."
The very specificity of this attack, however, is part of what makes the new findings important. Drugs that could prevent or reduce oxidative attack on these most vulnerable sites in a cell might have value against a wide range of diseases.
"Most people think of things like heart disease, cancer, aging, liver disease, even the damage from spinal injury as completely different medical issues," Beckman said. "To the extent they can often be traced back to inflammatory processes that are caused by oxidative attack and cellular damage, they can be more similar than different. It could be possible to develop therapies with value against many seemingly different health problems."
Beckman has spent much of his career studying the causes of amyotrophic lateral sclerosis, and this study suggested the processes outlined in this study might be relevant both to that disease and spinal cord injury.
Key to this research were new methods that allowed researchers to genetically engineer nitrotyrosine into HSP90. This allowed scientists to pin down the exact areas of damage, which may be important in the identification of drugs that could affect this process, the researchers said.














