HIV antibodies that are worth the wait
An effective vaccine against HIV-1 remains elusive, but one promising strategy focuses on designer antibodies that have much broader potency than most normal, exquisitely specific antibodies. These broadly neutralizing antibodies (bNAbs) can handle the high mutation rate of HIV particles that makes normal, very specific antibodies useless within a short space of time. A study published by Cell Press on March 28th in the journal Cell reveals surprising mutations in these antibodies that are crucial for strong protection against HIV-1. The findings could guide efforts to design better HIV-1 vaccines.
"This study demonstrates a fundamental aspect of antibodies' function and development that was not fully appreciated before," says study author Ron Diskin of the Weizmann Institute of Science. "We show that it will be important to pay more attention to previously ignored regions of antibodies to design effective vaccines."
Scientists have recently found that some HIV-1-infected individuals produce bNAbs naturally several years after infection. Animal studies have shown that these antibodies are very effective at protecting against and controlling HIV-1 infection, but what makes them so effective was unknown. Antibodies are Y-shaped molecules, and most variation is found at the two tips of the Y, called the complementarity determining regions, where antibodies make direct contact with the virus. On the other hand, relatively few mutations have been found in framework regions (the bottom half of the Y), which maintain the structural integrity of the antibody. Until now, the role of framework region mutations had been unclear.
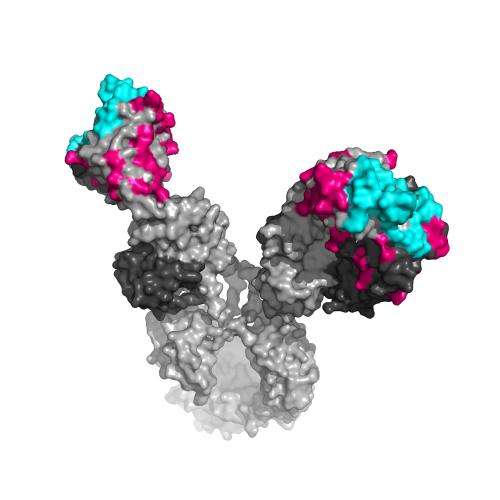
The study, led by Michel Nussenzweig of Rockefeller University and Pamela Bjorkman of the California Institute of Technology, has revealed that HIV-1-fighting bNAbs accumulate mutations in framework regions, in contrast to most antibodies. Surprisingly, these mutations strengthened the antibodies' antiviral activity while conserving key structural features. The researchers suggest that several years are required for infected individuals to produce these potent antibodies because it takes time for the right combination of various mutations to accumulate.
"Our study shows that the immune system has a variety of ways to make effective antibodies and that mutations in antibody framework regions, which are usually not changed when antibodies mutate to increase their efficacy, are required for anti-HIV antibodies," Bjorkman says. "This has clear implications for efforts to raise effective antibodies for the next generation of HIV vaccines."
Dr. Nussenzweig will be speaking at "What Will It Take To Achieve an AIDS-free World?"—the inaugural translational medicine conference on HIV research organized by Cell and the Lancet, which will bring the audiences and Editors of the Lancet and Cell together to bridge the gap between clinicians and researchers focused on understanding, managing, preventing, and curing HIV/AIDS. The meeting is in San Francisco on November 3-5, 2013. To view the program, submit an abstract, or register for the meeting, visit the website: http://www.translationalmedicine-lancet-cell.com/HIV/index.html.