The Parkinson's puzzle: Developing an assay to identify components in protein structures to aid diagnosis, treatment
As part of a new initiative to speed the search for changes in the body that can help predict, diagnose, or monitor Parkinson's disease, a research team led by Pacific Northwest National Laboratory recently received a grant from the National Institute of Neurological Disorders and Stroke (NINDS). Scientists from PNNL, University of Miami, Baylor College of Medicine, and Rush University have teamed to identify new components of the Lewy bodies that accumulate in the brain during Parkinson's, and then use ultra-sensitive methods to see if any of these proteins have leaked into cerebrospinal fluid or blood.
Parkinson's disease is a movement disorder that affects about 1 million people in the United States. Symptoms of the disease get worse over time, and include uncontrollable shaking, rigidity, slowed movements, and impaired balance.
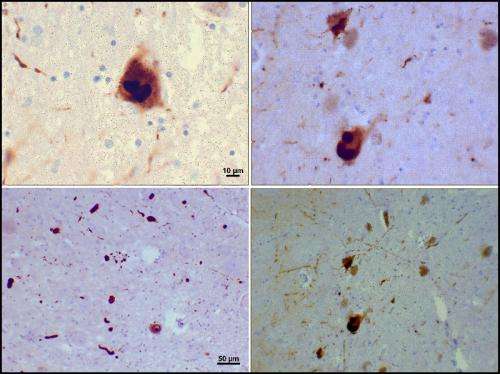
"Lewy bodies are abnormal protein aggregates that form in the nerve cells of Parkinson's disease patients," said PNNL biochemist Dr. Vladislav Petyuk, principal investigator of this 3-year, $900K project. "Their presence is one of the signature signs of the disease's progression. Unfortunately, right now, their presence can only be determined after a person has died, because it requires direct examination of brain tissue under the microscope."
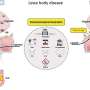
The team plans to develop a Lewy body assay based on biofluid protein measurements. They will use proteomics data obtained from brain tissue samples from 500 deceased individuals in studies conducted by Rush University. Differentially abundant proteins exclusively expressed in the brain tissue will be targeted for follow-up testing in easily obtained biofluids.
Detection of Lewy bodies in living humans could allow direct and accurate diagnostics of the disease's onset and progression. It would also act as a surrogate endpoint for assessing drug efficacy during clinical trials. The availability of a minimally invasive test capable of detecting Lewy bodies in living individuals would constitute a significant and welcome development for both clinical diagnostics and drug trials.
"The availability of brain tissue, cerebrospinal fluid, and blood from the same individuals allows us to directly explore the relationship between protein abundance profiles in brain tissue and biofluids," said Petyuk.
Aiding the team in this exploration will be an ultra-sensitive selected reaction monitoring approach developed by PNNL scientists Dr. Wei-Jun Qian and Dr. Tujin Shi of the Biological Sciences Division and in EMSL, a national user facility located at PNNL. They will also use other mass spectrometry capabilities developed at PNNL to reach even lower levels of quantitation. The information will be used to develop a biofluid-based statistical model that predicts the Lewy body load. They will validate the model by acquiring blood serum measurements for an independent Parkinson's disease case/control cohort based on subjects enrolled in another study at Rush.
"The main innovation of our research lies in our approach for testing our assumption that cerebrospinal fluid and blood bear the footprint of brain protein abundances, though at very low concentrations," said Petyuk. "If our hypothesis turns out to be true, especially for blood, this brain-biofluid protein correlation will open an avenue for developing biomarkers of other neurodegenerative disorders."