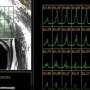
Novel small molecules used to visualize prostate cancer
Two novel radiolabeled small molecules targeting prostate-specific membrane antigen (PSMA) have excellent potential for further development as diagnostic and therapeutic radiopharmaceuticals, according to research published this month in The Journal of Nuclear Medicine. The imaging agents—123I-MIP-1072 and 123I-MIP-1095—were shown to have a high sensitivity of lesion detection in bone, soft tissue and the prostate gland with minimal retention in non-target tissue.
An estimated 238,500 men will be diagnosed with prostate cancer in 2013, and 29,700 will die from the disease. Accurate diagnosis and staging of prostate cancer is critical to determining appropriate patient management. Patients with localized disease may benefit from a curative treatment, while those with bone metastases are typically treated with systemic therapy.
"Current imaging techniques have limitations in diagnosing and staging prostate cancer. New imaging approaches, including the radiolabeled small molecules 123I-MIP-1072 and 123I-MIP-1095, may assess disease status more accurately," said John J. Babich, PhD, lead author of the article "First-in-Man Evaluation of Two High-Affinity PSMA-Avid Small Molecules for Imaging Prostate Cancer." Babich continued, "Improved imaging approaches could better facilitate the selection of optimal treatment and improve patient outcomes."
Separate studies were conducted as part of phase 1 trials under an investigational new drug application to measure the potential effectiveness of the small molecules in diagnosing and staging prostate cancer. In the first study, seven patients with documented prostate cancer were administered doses of 123I-MIP-1072 and 123I-MIP-1095 two weeks apart. In the second study, six healthy volunteers received 123I-MIP-1072 only. Whole body planar imaging and single photon emission computed tomography (SPECT)/computed tomography (CT) were performed for each group, and pharmacokinetics, tissue distribution, excretion, safety and organ radiation dose were analyzed.
Both 123I-MIP-1072 and 123I-MIP-1095 visualized lesions in soft tissue, bone and the prostate gland as early as one to four hours after injection. The imaging agents cleared the blood in a biphasic manner; however, clearance of 123I-MIP-1072 was approximately five times faster, resulting in a higher lesion-to-background ratio as compared to 123I-MIP-1095. The largest organ-absorbed radiation doses for 123I-MIP-1072 were to the urinary bladder, salivary glands, and kidneys; for 123I-MIP-1095 the absorbed doses to the salivary glands, kidneys and thyroid were the largest. Both imaging agents were well tolerated by the study population.
As a result of the phase 1 findings, 123I-MIP-1072 was evaluated as a diagnostic agent in subsequent clinical trials on the basis of its higher lesion-to-background ratios and prolonged tumor retention. 123I-MIP-1095 will be clinically evaluated for radiotherapy for metastatic prostate cancer as the 131I-labeled analog.
"A more accurate method of imaging prostate cancer and prostate cancer metastases would significantly impact the clinical management of men with prostate cancer. This would provide greater certainty as to the presence and extent of disease during the course of the patient's treatment," said Babich. "Data indicate that PSMA is an excellent target for molecular imaging of prostate cancer and that radiolabeled small molecules, which bind PSMA with high affinity, can localize prostate cancer anywhere in the body. The use of SPECT for molecular imaging could represent a significant advance in cancer evaluation."
More information: "First-in-Man Evaluation of Two High-Affinity PSMA-Avid Small Molecules for Imaging Prostate Cancer" The Journal of Nuclear Medicine.