Special CT improves radiotherapy planning
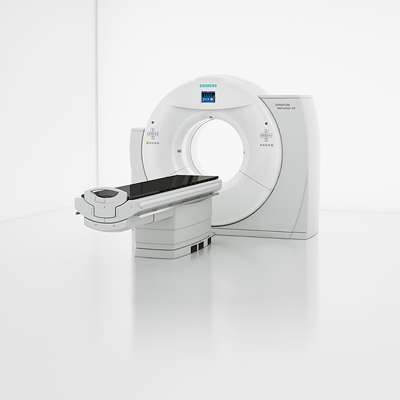
A computer tomograph (CT) with special software solutions is helping to improve the planning of radiotherapy, thus making cancer treatment more effective. Radiotherapy aims to irradiate tumors as precisely as possible. To make this possible, radiotherapists first make CT images to determine the exact size and location of the area to be irradiated. However, image quality is impaired by metal implants and breathing movements, thus making therapy planning more difficult. To counter these problems, the Siemens tomograph SOMATOM Definition AS Open RT Pro edition is equipped with software that offsets the effects of such interference so that the radiation can be more precisely targeted. The device has been equipped with a number of special features to enhance it for use in radiotherapy.
When making CT scans, the radiation penetrates metal implants such as artificial joints, pacemakers, and dental fillings only partially or not at all. As a result, metal artifacts appear as obstructions in the images. That's why the Siemens CT is equipped with the MARIS (Metal Artifact Reduction in Image Space) function, which reduces these artifacts in order to generate clear images. To do so, a corrective algorithm uses a two-dimensional value table to calculate the interference created by the metal objects and then eliminates these effects from the image. MARIS offers doctors five variously corrected images, from which users can select the one that is best suited for contouring the tumor.
In the device, Siemens is also making the benefits of dual-energy computer tomography available to radiotherapy for the first time. Dual-energy CT imaging makes two sequential scans at different energy levels and then combines them into a single dataset. Dual-energy images can be used to further reduce metal artifacts or accurately assess tissue density - and thus to calculate the optimal dose.
Breathing particularly causes tumors in the lung to change their position. With the Motion Management Pro module, the SOMATOM Definition AS Open RT Pro edition can analyze tumor motion during the breathing cycle. This allows the therapist to adjust the irradiation volume to the motion and only carry out the irradiation during specific phases of the breathing cycle, for example.