Burden of futile care in ICU studied: Patients waiting for care affected negatively, study presented
Researchers at UCLA studied the opportunity costs of providing futile care to patients in the ICU, finding that care was delayed or compromised for waiting patients when futile care was being provided in a full ICU. Futile treatment was identified by critical care specialists as ICU care from which patients could never receive a benefit, prolonged the dying process, or where the burdens far outweighed the benefits.
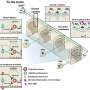
On a daily basis for a period of 3 months, researchers surveyed critical care physicians in five ICUs in one health-care system to identify patients receiving futile treatment. On days when the ICU was full and when there was at least one patient in the unit receiving futile treatment, they evaluated the number of patients who had to wait in the ED for more than 4 hours before being transferred to the ICU, as well as the number of patients who waited for more than one day to be transferred to the ICU from outside hospitals.
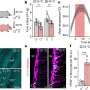
During the study, 36 critical care specialists made 6,916 assessments on 1,136 patients. There were 464 daily assessments of futile treatment (123 patients, 11% of all patients). There were 72 days when the ICU was full and had at least one patient receiving futile treatment. During those days, 33 patients waited in the ED for over 4 hours after it was determined that they required ICU-level care. Of the 22 patients who had to wait for more than one day to be transferred from an outside hospital, nine spent 16 days waiting when the ICU was full and contained at least one patient who was receiving futile treatment. Of the 37 patients who never transferred from an outside hospital, two died while waiting.
"We found that the burdens of futile treatment extend beyond the patients receiving that treatment," said Thanh Huynh, MD, a specialist in critical care medicine and pulmonology at UCLA. "We need to explore new ways to reorient treatment so that appropriate treatment is available to all patients."