Cataract surgeries on the rise as boomers age, raising access, cost issues
As baby boomers enter their retirement years, health care costs for complex and debilitating conditions such as Alzheimer's disease are expected to soar. Not drawing as much attention is the likelihood of similarly rising expenses for common age-related medical procedures. A Mayo Clinic study looked at one of those—cataract surgery— and found that more people are getting the vision-improving procedure, seeking it at younger ages and having both eyes repaired within a few months, rather than only treating one eye. The demand shows no sign of leveling off, raising the need to manage costs and ensure access to appropriate cataract treatment, the researchers say.
The findings are published in the Journal of Cataract & Refractive Surgery.
"Cataract surgery rates are rising in all age groups between 50 and 90, but the greatest increase is in the 70- and 80-year-olds. And part of that is that our older population, or the aging baby boomers, are working longer, they want to be more active, they have more demands on their vision," says senior author Jay Erie, M.D., a Mayo Clinic ophthalmologist. "That's why they're looking for surgery sooner—so that they can remain independent, remain active, continue to work."
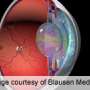
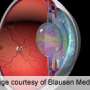
Cataracts can blur vision and worsen glare from lights. They can make it difficult to drive safely, perform household tasks and maintain a normal level of independence. In cataract surgery, the eye lens is removed and usually replaced with an artificial lens, without requiring a hospital stay. In the United States, age-related cataracts affect at least 22 million people and cost an estimated $6.8 billion to treat each year; the cataract caseload is expected to rise to 30 million people by 2020, the researchers noted.
Despite the common nature of cataracts, the U.S. has little current population-based data on cataract surgery, information that can help estimate demand. For the Mayo study, researchers mined the National Institutes of Health-funded Rochester Epidemiology Project to identify cataract surgeries in Olmsted County, Minn., from 2005-11. The project, a partnership of Mayo Clinic, Olmsted Medical Center and other health providers, makes the county one of few places worldwide where researchers can examine medical data on virtually everyone to see how often conditions strike and whether treatments succeed.
The research found:
- Cataract surgery has increased steadily, peaking in 2011 at a rate of 1,100 per 100,000 people.
- Sixty percent of people receiving cataract surgery on one eye returned within three months to have it performed on the second eye, a significant increase over the number in a previous Mayo study, which covered 1998 to 2004.
- The mean annual rate of cataract surgery for women was significantly higher than for men.
- There were significant increases in cataract surgery over the past 32 years among people in all age groups, except those 90 and older.
The trend raises questions about treatment costs and the resources needed to meet demand, Dr. Erie says. Medicare, for example, typically covers cataract surgery for its patients; in general, cataract surgery on a Medicare patient costs roughly $3,000 per eye.
"Ophthalmology and ophthalmologists and patients and payers are beginning to look at ways they can weigh the visual benefits to the individual patient against the cost to society as a whole … How can we maximize the outcome and minimize the cost to society?" Dr. Erie says.