Direct induction of chondrogenic cells from human dermal fibroblast culture by defined factors
A research team led by Professor Noriyuki Tsumaki of the Center for iPS Cell Research and Application (CiRA) at Kyoto University and Dr. Hidetatsu Ohtani, a former CiRA member who now works as a post doctoral fellow at Osaka University Graduate School of Medicine, has succeeded in directly converting human dermal fibroblasts into induced chondrogenic cells (iChon cells) without passing through an iPS cell stage in a process known as direct reprogramming. This finding has been published in PLOS ONE on October 16, 2013.
Articular cartilage, which is made up of chondrocytes and extracellular material in the form of Type II, Type IX, and Type XI collagens and aggrecan, fulfills the functions of ensuring smooth joint movement and absorbing shocks. Cartilage has little regenerative capacity and is gradually lost due to injury, aging, and other factors.
Normal articular cartilage consists of hyaline cartilage, but when this is lost it is partially replaced by fibrous cartilage. Fibrous cartilage produces Type I collagen and loses the extracellular material structure specific to cartilage. To restore cartilage function, this means that either high-purity hyaline cartilage not containing fibrous cartilage must be prepared and transplanted into the site where cartilage has been lost, or fibrous cartilage must be converted in situ into hyaline cartilage.
One conceivable method of producing cartilage would be to induce it from iPS cells. Alternatively, if it were possible to convert fibroblasts directly into chondrocytes without an intermediate iPS cell stage, chondrocytes could probably be produced in a shorter period of time than via an iPS cell-based method.
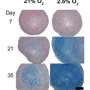
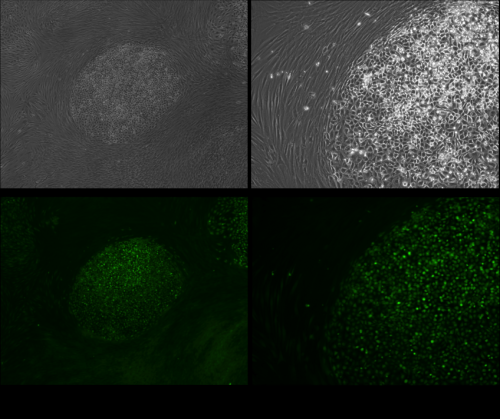
In 2011, Professor Tsumaki and his team reported that, by inserting into mouse dermal fibroblasts two reprogramming factors (c-MYC and KLF4) and one cartilage factor (SOX9), they had achieved direct reprogramming into induced chondrogenic cells without passing through an iPS cell stage. In the present study, the team confirmed that, by inserting the same three factors (c-MYC, KLF4, and SOX9) into human dermal fibroblasts, it was possible to directly generate iChon cells (Fig. 1). The iChon cells had lost the gene pattern specific to fibroblasts and instead displayed the gene pattern of chondrocytes. Additionally, when the iChon cells were transplanted to immunodeficient mice, they generated hyaline cartilage tissue (Fig.2), and no formation of teratomas or other tumors was observed for three months after the iChon cells were transplanted.
The present study demonstrates that direct reprogramming of fibroblasts into chondrocytes is also possible in human cells. Because the method used in the study makes use of c-MYC, which is thought to have a major role in tumorigenesis, and because it employs a retrovirus to introduce the factors, it could not be applied without modification in human therapy.
To produce chondrocytes for cartilage regeneration, CiRA also has the option of using the iPS cell stock which it is now engaged in building. Using the iPS cell stock would involve not autologous transplantation but isogeneic (allogeneic) transplantation, and rejection reaction and other risks would therefore need to be considered, but it would also have major cost benefits.
Another application of direct reprogramming is to carry out direct reprogramming of fibrous cartilage into hyaline cartilage in vivo. For this purpose, scientists will need to develop a technology to induce local reprogramming around cartilage tissue that avoids gene transduction, for instance by using chemical compounds instead. Going forward, a careful distinction will need to be drawn in applying the two methods – use of the iPS cell stock and use of the direct reprogramming method.
The researchers hope that the technique developed in this study will represent one option for supply of high-purity chondrocytes for cartilage regeneration, and that it will contribute to elucidation of the pathology of cartilage-related diseases.