The benefits of a spotless mind
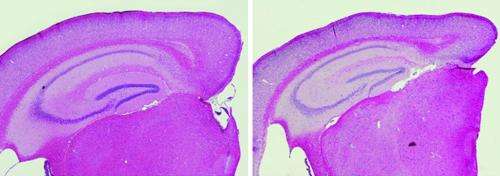
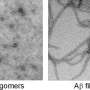
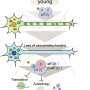
Alzheimer's disease is an age-related memory disorder characterized by the accumulation of clumps of the toxic amyloid-β (Aβ) protein fragment in the extracellular space around neurons in the brain. Drugs that help to 'clean up' cells by inducing autophagy—the degradation of unnecessary cellular components—are known to lower Aβ levels within cells and have been shown to rescue memory deficits in mice. A team of researchers including Per Nilsson and Takaomi Saido from the RIKEN Brain Science Institute have now found that autophagy also plays an important role in secreting Aβ from the cell into the extracellular space.
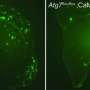
The researchers set out to investigate what would happen to extracellular Aβ aggregates, called plaques, when genetic methods were used to eliminate the autophagy process. They started with transgenic mice commonly used as a model for Alzheimer's disease. These mice have high levels of Aβ and Aβ plaque accumulation in their brains, and display learning and memory deficits. Surprisingly, in genetically engineered variants of these mice lacking autophagy-related gene 7 (Atg7), which is required for normal autophagy, the researchers found fewer extracellular Aβ plaques in the brain; instead, the Aβ seemed to accumulate inside the neurons. Conversely, increasing the expression of the Atg7 protein in neurons grown in cell culture resulted in an increase in the release of Aβ from the cells into the tissue culture medium. The findings suggest that autophagy is required for the secretion of Aβ from neurons into the extracellular environment.
Mice with an elevated expression of Aβ but defective autophagy seemed to have degenerated brain structures, as well as sicker neurons—as defined by their expression of markers of cell death—and worse learning and memory functions than mice with high Aβ expression but normal autophagy. This result indicates that autophagy is important for maintaining normal neuronal function and cognition in Alzheimer's disease. Moreover, because autophagy lowers Aβ levels within the cell, the researchers deduced that intracellular Aβ may be more toxic than extracellular Aβ with respect to inducing neuronal dysfunction and memory impairment.
The findings suggest that the effectiveness of therapeutic strategies for Alzheimer's disease may be improved by targeting the elimination of intracellular Aβ deposits rather than extracellular plaques. "Intraneuronal Aβ accumulation is seen in early Alzheimer's disease in humans, similar to what we found upon autophagy deletion in mice," explains Nilsson. "Targeting this pool of Aβ may therefore offer a potential treatment for Alzheimer's disease," he says.
More information: "Aβ Secretion and Plaque Formation Depend on Autophagy," Nilsson, Krishnapriya Loganathan, Misaki Sekiguchi, Yukio Matsuba, Kelvin Hui, Satoshi Tsubuki, Motomasa Tanaka, Nobuhisa Iwata, Takashi Saito, Takaomi C. Saido. Cell Reports - 17 October 2013 (Vol. 5, Issue 1, pp. 61-69) DOI: 10.1016/j.celrep.2013.08.042