Genetics contribute to increased risk for end-stage renal disease for African Americans with chronic kidney disease
In the United States, African Americans have approximately twice the risk of end-stage renal disease compared to white Americans, despite a similar prevalence in earlier stages of chronic kidney disease. A large study co-authored by George Washington University (GW) researcher Dominic Raj, M.D., identifies factors that mediate differences in the progression of chronic kidney disease between black patients and white patients, as well as among black patients, in order to reduce the excess burden of end-stage renal disease and its complications in black patients.
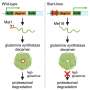
The findings, published in the New England Journal of Medicine, examines the effects of variants in the gene encoding apolipoprotein L1 (APOL1) on the progression of chronic kidney disease, according to whether patients have two copies of high-risk APOL1 variants (APOL1 high-risk group) or zero or one copy (APOL1 low-risk group). Renal risk variants in APOL1 were associated with higher rates of end-stage renal disease and progression of chronic kidney disease that were observed in black patients as compared with white patients, regardless of diabetes status.
The findings came from two large National Institutes of Health-funded study cohorts of nearly 5,000 individuals with kidney disease, including the African American Study of Kidney Disease and Hypertension (AASK) and the Chronic Renal Insufficiency Cohort (CRIC) study. The study was supported, in part, by a recent R0-1 grant awarded to Raj.
"This study is a unique example of the importance of collaboration across institutions to deliver high quality science," said Raj, director of the division of nephrology and professor of medicine at the GW School of Medicine and Health Sciences.
The AASK study, which enrolled African American patients with chronic kidney disease attributed to hypertension, found that kidney failure occurred in 58.1 percent of patients in the APOL1 high-risk group and 36.6 percent of those in the APOL1 low-risk group. In the CRIC study, kidney function decline was greater among black patients in the APOL1 high-risk group, but it was similar among black patients in the APOL1 low-risk group and white patients, regardless of their diabetes status.
"This study shows that APOL1 variant confers risk for progression of kidney diseases, independent of blood pressure control and diabetic status in African Americans. Chronic kidney disease is one of the most glaring examples of racial and ethnic disparities in health outcomes in the United States," said Raj. "While this is an important contribution that furthers our understanding for the cause for such disparity, this study also highlights the need for further studies that could lead to risk stratification and early and targeted interventions."
More information: "APOL1 Risk Variants, Race, and Progression of Chronic Kidney Disease," www.nejm.org/doi/full/10.1056/NEJMoa1310345