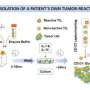
New data for engineering immune cells shows early promise in solid tumors
Engineered immune cells, called CARTmeso cells, designed to direct antitumor immune responses toward tumors that carry a protein called mesothelin, showed antitumor activity in two patients with advanced cancers that had not responded to prior treatments, according to a study published in Cancer Immunology Research, a journal of the American Association for Cancer Research.
Chimeric antigen receptor T cells (CAR T cells) are a form of personalized cell therapy that uses immune cells called T cells from patients. After T cells are harvested from a patient, they are engineered to bear a molecule that allows them to attach to a specific protein carried by the patient's cancer cells and to be triggered to kill the cancer cells when they do so. CAR T cells have shown early promising results for patients with some types of leukemia and lymphoma; however, they have not been very successful for solid cancers, one of the major issues being toxicity. Because normal cells express the CAR T cell target protein, albeit at lower levels than cancer cells, the engineered T cells recognize and attack the normal cells as well the cancer cells, causing off-target toxicity.
"So far, researchers have been permanently modifying T cells by using a variety of methods, including using viruses," said Carl H. June, M.D., a professor of pathology and laboratory medicine in the Perelman School of Medicine at the University of Pennsylvania and director of translational research in the university's Abramson Cancer Center.
"We engineered T cells to express a CAR for about three days, after which the mRNA is metabolized rapidly by the system, so the T cells basically revert to what they were before in the patient," explained June. "These T cells recognize a protein called mesothelin present in many tumors, including mesothelioma and pancreatic cancers, hence we named them CARTmeso cells. Our strategy is to give multiple infusions of CARTmeso cells to the patient, and if there is toxicity, we could abort the toxicity just by stopping the infusions, because the mRNA-based CARs rapidly revert to normal T cells."
"We found that the temporary CARs we engineered are safe, with no significant on-target, off-tumor toxicity," June added. "We have evidence of antitumor effects in two patients whose advanced tumors failed previous therapies. These results, albeit preliminary, are very promising."
June and colleagues recruited two patients, ages 75 and 81 years, to a phase I clinical trial. One patient had advanced mesothelioma, and the other patient had metastatic pancreatic cancer that progressed after failing first-line therapy. The objective of this trial was to evaluate the manufacturing feasibility and safety of the mRNA-based CARTmeso cells. The researchers isolated T cells from the patients, reproduced them in large numbers in the laboratory, and engineered them to recognize mesothelin on tumor cells, using a biological material called mRNA. After ensuring viability and specificity of the engineered cells, the researchers infused the patients' modified T cells back into their bodies.
After receiving three infusions of CARTmeso cells, the patient with mesothelioma showed stable disease, as evaluated by imaging. The patient with pancreatic cancer received eight infusions of CARTmeso cells, and fluid collected from his abdomen showed a 40 percent decrease in the number of tumor cells that expressed mesothelin. The researchers evaluated additional tumor markers and confirmed antitumor activity.
"We found that these CARTmeso cells not only have antitumor activity, but also act like a vaccine, and trigger a response against the patient's own tumor," said June. "This new form of CAR therapy provides a new tool to evaluate CAR therapies for solid cancers."
Adverse events observed during the trial include an anaphylactic reaction and an intestinal obstruction.