Nursing methods seek rural health care improvements
It's not a matter of numbers but location.
With 1,247 registered nurses per 100,000 people, South Dakota has one of the nation's highest ratios of registered nurses, according to the 2013 U.S. Nursing Workforce Report.
"One would assume with South Dakota's larger population ratio of nurses that our state would have our needs met. However, some rural areas have difficulty finding nurses, while some areas, such as Minnehaha and Pennington counties, may have more than an adequate supply," explains Linda Young, nursing specialist at the South Dakota Board of Nursing.
Location makes a difference
The South Dakota Board of Nursing does not monitor where these nurses work but where they live. Young reports that as of December 2012, 13,307 registered nurses reside within South Dakota. However, they don't necessarily work in the town where they live.
"When we break that down by county or region, we have those pockets where there aren't enough nurses to meet the needs of those in the communities," Young explains. She cites the central region, from Corson County to Gregory County, which has numbers ranging from 9 to 77 nurses per county.
South Dakota State University's Lois Tschetter, an associate professor in nursing, seeks to improve these statistics.
She is project director for a three–year, $1.09 million grant from the U.S. Department of Health and Human Services that has positioned the nursing program at the forefront of efforts to prepare students to work in rural settings.
For her work, Tschetter was named Researcher of the Year for the SDSU College of Nursing at the 2013 Celebration of Faculty Excellence in February.
The Simulation, Informatics and Technology Enhancement (SITE) project began in July 2011. Nancy Fahrenwald, dean and former associate dean for research; instructor Paula Lubeck, who is the project manager, and 10 faculty members in the areas of mental health, pediatrics and medical surgical nursing have been working on the project.
Rural nursing present challenges
"It's a different type of nursing," says Young of the challenges that rural health care presents.
Nurses in these communities have to know all aspects of health care, Tschetter explains. A pregnant woman may come into the rural hospital emergency room in labor and the nurse must simultaneously provide emotional support to the patient and her family as well as collect assessment data and communicate with the physician regarding a plan for care.
"If you come to small facility and build your skill set, you'll be able to work anywhere," says Carmen Fees, director of nursing at the Philip Health Services. Philip is 80 miles east of Rapid City and 80 miles southwest of Pierre.
Affiliated with the Rapid City Regional Hospital, Philip Health Services has an 18-bed hospital and 30-bed nursing home. More than half of the hospital patients are waiting for a long-term care bed, and nursing home beds are filled as soon as one is available, Fees explains. The two facilities share nurses.
"Just one person with enthusiasm, positive attitude and a skill set can make a huge difference here," Fee says, but there's a lot of responsibility.
"If you are the nurse on the floor, you are the respiratory therapist, the IV person and the wound care specialist," Fees explains. "You get to run the whole show."
That attracts some nurses, but frightens others, especially those fresh out of nursing school.
Simulations re-create rural scenarios
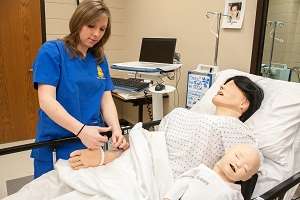
Through the grant, the SDSU research team built a simulation lab on the third floor of Wagner Hall in which nursing students can learn the wide of range of skills they will need, according to Tschetter. Pediatric and infant mannequins were purchased to go with the four adult mannequins the college already owned.
Instructors have developed simulations to mimic situations students could encounter and implemented them into the curriculum, Tschetter explains. One setting might be a rural clinic, another in a rural hospital and a third in a large acute-care setting.
Someone comes into a small 20-bed hospital, for instance, Tschetter says, "and the nurse will have to use telemedicine to call providers at a large health-care institution where experts can provide guidance on how to care for this patient." Nursing students work through the scenarios using the lab mannequins, review the videotape with their instructors and then discuss what went well and how they can do better in the future."
Students can have experiences that they wouldn't get to be a part of in the hospital," Tschetter says. "And it's safe; no one gets hurt."
Young sees this type of training as beneficial to new graduate nurses. "To give them additional education and training opportunities while still under the wing of experienced licensed nurses will give them the confidence and competency they need."
Curriculum to help rural health care nationwide
As part of the grant, Tschetter and her team will share what they've learned with other nursing schools so they can develop programs specifically geared to rural health care. "We can help them get that rural focus for their students," Tschetter says.
More recently, the simulations have involved pharmacy students, adding the collaboration emphasized nationally, she explains. With future funding, the researcher hopes to add SDSU students from nutrition and social work to the scenarios. "We think our rural focus is unique and something we want to pull together, write about and make available to other schools," Tschetter explains. SDSU has implemented this curriculum in Brookings, Sioux Falls and Rapid City and will extend this to its new site in Aberdeen.
Based on her experience with the board of nursing, Young says, "Every one of the states has a rural nature to it, and all deal with these same rural issues."
As a result of this research, the curriculum that Tschetter and her team have developed at SDSU has the potential to improve health care for rural populations across the nation.













