Heart attack survivors paint a complex picture of adhering to medicine
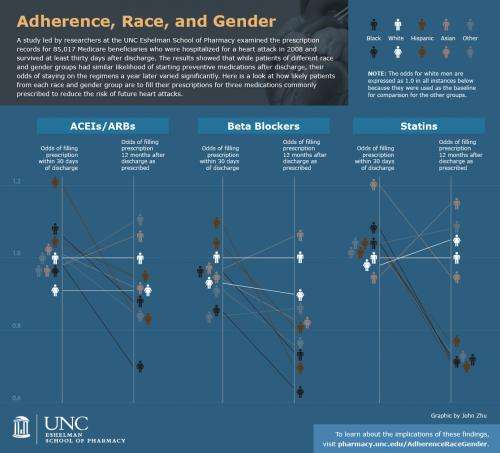
Heart attack survivors of different races and genders are about equally likely to be on medications that reduce the risk of another heart attack and other potentially life-threatening cardiovascular problems. But according to a new study at the University of North Carolina at Chapel Hill, that's not the case a year later. The odds that an patient is still taking the medications as prescribed within a year vary significantly depending on race and gender, and black and Hispanic women are the least likely to adhere to their regimens.
The work, led by Gang Fang at the UNC Eshelman School of Pharmacy, suggest that while national initiatives have been effective in encouraging clinicians to prescribe preventive medications for heart-attack patients at the time of discharge, more needs to be done to help patients stay on those medications.
Fang and his team examined prescription records and looked at three types of medications—statins, beta blockers and ACEIs/ARBs— for more than 85,000 Medicare Part D beneficiaries who were hospitalized for a heart attack in 2008 and survived at least 30 days after discharge. The results, published last month in the journal Circulation, show that although there is little racial and gender disparity in getting the patients started on preventive medications, keeping them on those medications long-term is a different story.
"Adherence is a two-dimensional behavior: The physician has to prescribe the medication, and the patient has to fill the prescription," said Fang, an assistant professor in the School's Division of Pharmaceutical Outcomes and Policy.
"The policy implication from our study is that we should now put a lot of emphasis on helping patients, especially minority groups, understand the importance of these medications and help them improve their long-term adherence to get the greatest benefits."
Julie Lauffenburger, a graduate student at the school and first author on the paper, said the findings also point to a need for different interventions for different groups.
"Some adherence interventions in the past have focused on a blanket approach to emphasizing adherence even though patient demographic subgroups may have different needs and perceptions about medication use," she said. "These results suggest that more targeted interventions need to be considered, especially for adherence after heart attacks."
Using white men as the reference group for comparisons, the study found adherence was worse among racial minorities.
- Black and Hispanic women were the least likely to be filling their prescriptions as prescribed in the year after discharge,
- black and Hispanic patients had the lowest likelihood of adherence to beta-blockers and statins,
- black patients had the lowest likelihood of adherence to ACEIs/ARBs
The study also found that women, who have worse outcomes than men after heart attacks, had worse adherence within each race group, especially in blacks and Hispanics. One possible explanation is a difference in men and women's beliefs on the severity of their heart attacks and the benefits from the medications.
The findings raise a number of other questions about what might influence adherence. For example, the study revealed different levels of adherence to each of the three medications within a race and gender group. White women, for instance, were more adherent to statins but less adherent to ACEIs/ARBs and beta-blockers.
"There is no clinical evidence that says one of these drugs is more important than the others," said Fang. "So this brings up a very interesting question about how clinicians and patients perceive benefits from each of the drugs."
The researchers also adjusted their results to control for out-of-pocket medication costs and whether the patients had a follow-up visit with a primary-care physician or a cardiologist. They did not find a significant connection between those factors and the racial and gender gaps in adherence.
"It's not just how much you pay for medications or whether you visit a primary-care physician or cardiologist after discharge," said Fang. "For instance, it could be whom you see—the quality of the providers' care and services."














