May 12, 2014 report
Study suggests lung microbiota promotes tolerance to allergens in neonates
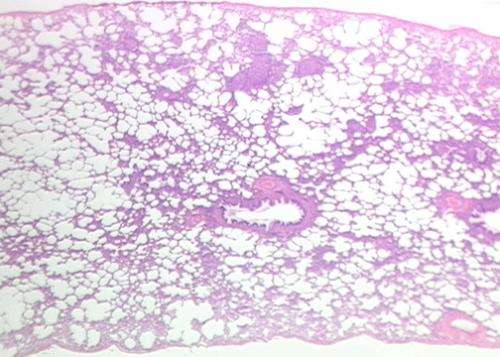
(Medical Xpress)—A study by a team made up of researchers from Switzerland and the U.K. has determined that lung microbiota in neonate mice promotes tolerance to allergens both early on and later in life. In their paper published in the journal Nature Medicine, the group reports on experiments they conducted in a lab that involved testing mice soon after birth for microbiota levels and types in the lungs and their tolerance to allergens.
Reports that over-cleaning a newborn's environment could lead to a compromised immune system have been surfacing in recent years and indeed some studies have found that children raised in near sterile environments tend to have more problems with asthma and other allergies as they grow older. In this new effort, the researchers sought to find a concrete connection between microbiota in the lungs of newborn mice, and their subsequent tolerance to allergens.
Mice (and humans) are born with sterile lungs, shortly after birth however, various forms of microbiota begin to take up residence, which in most cases, is believed to help ward off allergens. The researchers in this study tested the mice in various ways. First, they tested allergen response immediately after birth, before microbiota had built up. Test results showed a high incidence of lung inflammation. At just two weeks old, the young mice had built up an impressive array of biota in their lungs, and testing showed, a marked increase in resistance to allergens. After two months, the mice showed a high degree of immune response to allergens. In another test, they kept some young mice in sterile environments, preventing microbiota build up in their lungs. When introduced to allergens, the older mice reacted in ways similar to newborns, i.e. they exhibited a high incidence of lung inflammation.
The researchers suggest their work indicates that microbiota play a major role in immune development in mice, and possibly in other mammals. They believe that because of what they found, that its more likely that such mammals would be more susceptible to asthma later on in life, and because of that, suggest that parents of newborns refrain from using antibacterial wipes and soaps, and instead use simple soap and water when washing up to allow their baby to develop an immunity at a very early age.
More information: Lung microbiota promotes tolerance to allergens in neonates via PD-L1, Nature Medicine (2014) DOI: 10.1038/nm.3568
Abstract
Epidemiological data point toward a critical period in early life during which environmental cues can set an individual on a trajectory toward respiratory health or disease. The neonatal immune system matures during this period, although little is known about the signals that lead to its maturation. Here we report that the formation of the lung microbiota is a key parameter in this process. Immediately following birth, neonatal mice were prone to develop exaggerated airway eosinophilia, release type 2 helper T cell cytokines and exhibit airway hyper-responsiveness following exposure to house dust mite allergens, even though their lungs harbored high numbers of natural CD4+Foxp3+CD25+Helios+ regulatory T (Treg) cells. During the first 2 weeks after birth, the bacterial load in the lungs increased, and representation of the bacterial phyla shifts from a predominance of Gammaproteobacteria and Firmicutes towards Bacteroidetes. The changes in the microbiota were associated with decreased aeroallergen responsiveness and the emergence of a Helios− Treg cell subset that required interaction with programmed death ligand 1 (PD-L1) for development. Absence of microbial colonization10 or blockade of PD-L1 during the first 2 weeks postpartum maintained exaggerated responsiveness to allergens through to adulthood. Adoptive transfer of Treg cells from adult mice to neonates before aeroallergen exposure ameliorated disease. Thus, formation of the airway microbiota induces regulatory cells early in life, which, when dysregulated, can lead to sustained susceptibility to allergic airway inflammation in adulthood.
© 2014 Medical Xpress

















