Different endotypes may lead to type 1 diabetes
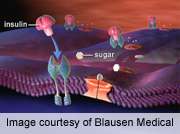
(HealthDay)—Different immunopathological processes may lead to the development of type 1 diabetes, according to research published online June 17 in Diabetes.
Sefina Arif, Ph.D., of the King's College London School of Medicine, and colleagues performed immunologic analysis of autoantibodies and autoreactive T-cell responses in blood from 33 children/adolescents newly diagnosed with type 1 diabetes. In addition, they performed immunohistological analysis of postmortem samples of islet tissue from 21 children/adolescents with recently diagnosed type 1 diabetes. The researchers explored evidence for different immunological phenotypes indicating disease heterogeneity in type 1 diabetes.
In blood analysis for the first cohort, the researchers observed two equal-sized patient agglomerations, characterized by pro-inflammatory (interferon-γ+, multi-autoantibody-positive) and partially-regulated (interleukin-10+, pauci-autoantibody-positive) responses. Similar clustering was observed in multi-autoantibody-positive siblings without diabetes at high risk of disease progression. Analysis of pancreatic tissue in the second cohort showed two types of insulitic lesion that differed by degree of cellular infiltrate and presence of B lymphocytes. Each subject had only one infiltration phenotype.
"These data indicate potentially related islet and blood autoimmune response phenotypes that coincide with, and precede disease," the authors write. "We conclude that different immunopathological processes (endotypes) may underlie type 1 diabetes, carrying important implications for treatment/prevention strategies."
More information:
Abstract
Full Text (subscription or payment may be required)
Copyright © 2014 HealthDay. All rights reserved.