Scientists discover new, readily available source of stem cells
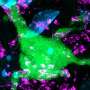
Scientists have discovered a new source of stems cells and have used them to create muscle, bone, fat, blood vessel, nerve and liver cells in the laboratory. The first report showing the isolation of broad potential stem cells from the amniotic fluid that surrounds developing embryos was published today in Nature Biotechnology.
"Our hope is that these cells will provide a valuable resource for tissue repair and for engineered organs as well," said Anthony Atala, M.D., senior researcher and director of the Institute for Regenerative Medicine at Wake Forest University School of Medicine.
Atala announced the breakthrough with colleagues from Wake Forest University School of Medicine and Harvard Medical School.
"It has been known for decades that both the placenta and amniotic fluid contain multiple progenitor cell types from the developing embryo, including fat, bone, and muscle," said Atala. "We asked the question, 'Is there a possibility that within this cell population we can capture true stem cells?' The answer is yes."
Atala and colleagues discovered a small number of stem cells in amniotic fluid –
estimated at 1 percent – that can give rise to many of the specialized cell types found in the human body. The scientists believe the newly discovered stem cells, which they have named amniotic fluid-derived stem (AFS) cells, may represent an intermediate stage between embryonic stem cells and adult stem cells. They have markers consistent with both cell types.
"It took this long to verify that we had a true stem cell," said Atala, who began the work seven years ago. "These cells are capable of extensive self-renewal, a defining property of stem cells. They also can be used to produce a broad range of cells that may be valuable for therapy."
An advantage of the AFS cells for potential medical applications is their ready availability. The report describes how the cells were harvested from backup amniotic fluid specimens obtained for amniocentesis, a procedure that examines cells in this fluid for prenatal diagnosis of certain genetic disorders. Similar stem cells were isolated from "afterbirth," the placenta and other membranes that are expelled after delivery.
Atala said a bank with 100,000 specimens theoretically could supply 99 percent of the U.S. population with perfect genetic matches for transplantation. There are more than 4 million live births each year in the United States.
In addition to being easily obtainable, the AFS cells can be grown in large quantities because they typically double every 36 hours. They also do not require guidance from other cells (termed "feeders") and they do not produce tumors, which can occur with certain other types of stem cells. The scientists noted that specialized cells generated from the AFS cells included all three classes of cells found in the developing embryo - termed ectoderm, mesoderm, and endoderm. In their high degree of flexibility and growth potential, the AFS cells resemble human embryonic stem cells, which are believed capable of generating every type of adult cell.
"The full range of cells that AFS cells can give rise to remains to be determined," said Atala. "So far, we've been successful with every cell type we've attempted to produce from these stem cells. The AFS cells can also produce mature cells that meet tests of function, which suggests their therapeutic value."
The functional tests included implanting neural cells created from AFS cells into mice with a degenerative brain disease. The cells grew and "re-populated" the diseased areas. In addition, bone cells produced from the stem cells were successfully used to grow bony tissue in mice, and liver cells were able to secrete urea, which the liver produces from ammonia.
The potential to generate a broad range of mature cell types is why many scientists believe stem cells have promise to replace damaged cells and tissue in conditions such as spinal cord injuries, diabetes, Alzheimer's disease and stroke.
Source: Wake Forest University Baptist Medical Center