Researchers have found a gene variant that can more than double the risk of developing the degenerative eye disease, age-related macular degeneration.
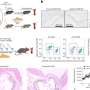
The macula lies at the centre of the retina and is essential for detailed central vision. Degeneration of the macula interferes with important tasks such as reading and driving.
Age-related macular degeneration (AMD), the cause of which is poorly understood, is the leading cause of visual loss in older people and the commonest cause of blindness in the USA and European countries.
The researchers based their findings on studies of patients with AMD (603 from England and 244 from Scotland) who were compared with 701 unaffected people.
They found that a variant in the complement C3 gene influenced the risk of developing AMD. For the 30% of the population who carry one copy of the so-called ‘fast’ variant the risk of AMD was increased by 70%, and for the 4% of people with two copies of the ‘fast’ variant the risk of AMD was more than doubled.
AMD can take two forms called ‘wet’ (also called choroidal neovascularisation or CNV) and ‘dry’ (also called geographic atrophy or GA). The ‘fast’ variant in the C3 gene increases the risk of both forms of the disease.
The complement C3 gene has a central role in the immune system. The results of this research provide strong evidence that inflammation is an important part of the disease process in AMD.
The goal of this type of research is to achieve a full understanding of the causes of AMD, which should lead to the development of better treatment and strategies for prevention of this common and debilitating disease.
Professor John Yates, at the University of Cambridge, said: “AMD is devastating for those who lose their site and we hope that a better understanding of what causes the disease will eventually lead to better treatment and perhaps prevention”.
The initial studies were carried out by a team of researchers led by Professor Yates and Professor Tony Moore at the UCL Institute of Ophthalmology. Further work to confirm the initial findings was carried out by researchers in Scotland led by Professor Alan Wright, Medical Research Council Human Genetics Unit, Edinburgh.
Source: University of Cambridge