Immune cells fighting chronic infections become progressively 'exhausted,' ineffective
A new study of immune cells battling a chronic viral infection shows that the cells, called T cells, become exhausted by the fight in specific ways, undergoing profound changes that make them progressively less effective over time.
The findings also point to interventions that would reverse the changes, suggesting that novel therapies could be developed to reinvigorate T cells that become depleted in their struggle against a virus. Alternatively, strategies that would intentionally trigger the immune-dampening mechanisms explored in the study could prove useful in countering autoimmune disorders in which the immune system is inappropriately activated.
Although the experiments were conducted in mice, the problem of T-cell exhaustion has also been identified in HIV, hepatitis B, and hepatitis C infections in humans, as well as some cancers, such as melanoma. A report on the study results appears in the current issue of Immunity, published online October 18.
“We knew that T cells responding to chronic infections become progressively compromised in many of their functional properties,” says E. John Wherry, Ph.D., an assistant professor in the Immunology Program at The Wistar Institute and lead author on the Immunity study. “Put simply, the T cells become exhausted as time passes. What we wanted to learn in our study was what the specific problems were with these cells and whether their depleted state could be reversed.”
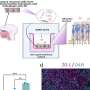
Using a technique called gene-expression profiling, Wherry and his colleagues identified 490 genes whose activity in T cells is altered during a chronic viral infection. Closer study at different time points using a 22-gene subset of the larger group of genes provided molecular signatures of progressive T-cell exhaustion. Only a few changes in the activity of the 22 genes were seen at the end of the first week of infection, increasing to 9 differences at two weeks, 18 differences at one month, and 21 differences at two months. At the end of two months, T cells contending with a chronic infection were sluggish metabolically and immunologically unresponsive to stimulus.
One gene identified as playing a central role in this process is called PD-1, which codes for an inhibitory receptor on the surface of the T cells. By blocking PD-1 in vivo, the researchers found they could alleviate T-cell exhaustion, get more functional T cells, and control the infection better.
“Blocking this one pathway partially reverses T-cell exhaustion in some settings, suggesting that we may be able to intervene to reinvigorate depleted immune cells,” says Wherry. “The T cells undergo many changes during chronic infections, however, so that it will be important to learn how to treat them for multiple problems.”
Wherry notes that the mechanisms involved in T-cell exhaustion also have important upsides.
“The flip side of this process is that the immune system has developed an effective way to turn off its response to a stimulus – which is exactly what one wants to do in the case of autoimmunity,” he says.
He points out, too, that the energy outlay during the acute phase of the immune system’s response to an infection is enormous – and fundamentally unsustainable.
“In the first week of an immune response to a virus, T cells can divide every four to six hours, as fast as any other mammalian cell at any time during development,” Wherry says. “In terms of their rate of division, T cells are in the same category as cells in the earliest stages of embryonic development. The energy involved in doing this is extraordinary, and the body can’t keep that up for an extended period of time.”
Source: The Wistar Institute