Researchers find key to stopping cancer in its tracks
University of Manchester researchers have discovered a key process that may be involved in the spread of cancer by studying the growth of human embryonic stem (ES) cells.
Dr Chris Ward and his team used the ES cells to investigate how some tumours are able to migrate to other parts of the body, which makes the treatment of cancer much more difficult. He believes his work could lead to new treatments and stop 80-90% of cancers in their tracks.
They studied a crucial change that makes cancer cells able to start moving and spread into other tissues.
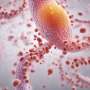
Normal cells, as well as early cancer cells, are called epithelial cells because they bind tightly to each other forming stable layers of tissue. However, as a tumour becomes more advanced some of the cells change to become 'mesenchymal'. Mesenchymal cells do not bind to each other, forming more disorganised tissues in which the cells can move around. Since this crucial change - known as the epithelial-mesenchymal transition - was first observed in the early embryo, Dr Ward theorised that embryonic stem cells might undergo a similar process.
The study, which was funded by the Association for International Cancer Research (AICR) and also involved the University's immunology group at the Paterson Institute for Cancer Research (PICR), found that the protein E-cadherin stopped cells from migrating during normal growth.
It also found that, as well as helping cells stick together, E-cadherin also blocked the action of another protein known to increase the mobility of cells. This important dual function of E-cadherin opens up the potential for new targets to prevent tumour cells from spreading.
Dr Ward, whose findings are published in the journal Cancer Research, said: "We have shown that ES cells spontaneously change in a manner that is remarkably similar to the epithelial-mesenchymal transition. They lose the proteins that cells use to bind to each other and have other protein alterations that are characteristic of spreading cancer cells.
"Since ES cells can be grown in the laboratory, where they keep the characteristics of the cells in the early embryo, they can be studied in detail. By studying these ES cells we have already identified a novel component of this transition process. We expect the use of ES cells will lead to the identification of other unknown factors involved in cancer cell spread, hopefully leading to new avenues for cancer therapy."
Previously, it has not been possible to study this crucial transition in patients since this would involve invasive techniques that may interfere with any treatment of the disease. Where excised tumour cells have been used, it is difficult to know if the cells were from the right area - i.e. the growing part of the tumour. The team's discovery that it happens spontaneously in ES cells means that it can be studied much more easily in the laboratory.
"Understanding how cancer cells start to spread is tremendously important for cancer research; tumours that do not spread are rarely dangerous," said Dr Ward, who leads the stem cell research group in the School of Dentistry.
"It is the ability of tumours to invade into other tissues and spread around the body that makes them so dangerous. Finding out more about the mechanism that controls the spread of cancer cells will help us find new treatments that can prevent tumours spreading and make them essentially harmless."
He added: "Previously we studied the process in mouse ES cells. When we used human ES cells, we found they had a similar response, which is very good news.
"Potentially, our findings can be applied to the most common form of cancer, carcinoma, found in the breast, lung and gut for example, which makes up 80-90% of all cancers."
Norman Barrett, Chief Executive of AICR, said: "The grant to support Dr Ward's work is given in line with the charity's policy of funding the most exciting and novel approaches to research worldwide. It is important to fund work that pushes the boundaries and Dr Ward and his team are pursuing research which could in future change the lives of tens of thousands of people in the UK and many more across the world."
Source: University of Manchester