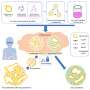
'Personalized' genome sequencing reveals coding error in gene for inherited pancreatic cancer
Scientists at the Sol Goldman Pancreatic Cancer Research Center at the Johns Hopkins Kimmel Cancer Center have used "personalized genome" sequencing on an individual with a hereditary form of pancreatic cancer to locate a mutation in a gene called PALB2 that is responsible for initiating the disease. The discovery marks their first use of a genome scanning system to uncover suspect mutations in normal inherited genes.
The findings, they say, underscore the value of so-called "personalized genome" sequencing, which decodes a person's genes and compares the changes to those found in healthy people. "Gene sequencing has always had the potential to help us learn if a person is susceptible to certain diseases," says Alison Klein, Ph.D., director of the National Familial Pancreas Cancer Tumor Registry at Johns Hopkins. "By finding the genetic error responsible for this patient's pancreatic cancer, our team has provided an excellent example of the power of this approach."
The coding error in PALB2, which stands for "partner and co-localizer of BRCA2" causes a shortened version of the protein encoded by this gene, rendering it incapable of working with another cancer-related gene, BRCA2, to repair broken DNA. Mutations in BRCA2 are also known to cause hereditary forms of cancer.
Klein and her team caution that their finding has not yet resulted in a clinical test for the hereditary pancreas cancer gene, but laboratories at Johns Hopkins and possibly elsewhere will be developing one, which she says can be used to increase cancer surveillance for early signs of disease in those at risk.
Reporting their findings in the March 5 edition of Science Express, the Johns Hopkins researchers say they sequenced genes taken from a person with pancreatic cancer whose sister also had the disease, suggesting an inherited predisposition. "Generally, we need data from very large families to identify the inherited gene, and that was not available in this case," says Siân Jones, Ph.D., research associate at the Johns Hopkins Kimmel Cancer Center. Instead, the investigators used high-powered computer software to scan all known protein-coding genes in the patient -- approximately 20,000 of them - to find more than 15,000 variations.
Most of the variations were normal ones coding for such things as eye or hair color, but the search was designed to track down particular mutations that caused certain proteins to be shortened, a process that commonly occurs in cancer, says James Eshleman, M.D., Ph.D., associate professor of pathology and oncology.
The search yielded one gene variant, PALB2, resulting from a substitution of a single DNA letter coding for cytosine with a different one that codes for thymidine.
The research team then scanned for the PALB2 gene in 96 other individuals with pancreatic cancer who each had at least one relative with pancreatic cancer. Three of them had coding errors in the PALB2 gene that shortened the protein in a similar way. She estimates that three percent of people with hereditary pancreatic cancer have mutations in PALB2, making it the second most common gene mutation in these patients after BRCA2.
The investigators believe that their approach could be used to identify inherited alterations that predispose people to other types of cancer as well as other genetic-based diseases. "The more information we have about normal variants, the easier it will be to find disease-causing ones," says Michael Goggins, M.D., professor of pathology, medicine and oncology at Johns Hopkins.
In the future, scanning genomes for hereditary disease-causing genes could become "reasonably routine," according to Bert Vogelstein, M.D., an investigator at the Howard Hughes Medical Institute and co-director of the Ludwig Center at Johns Hopkins.
The investigators say that the cost to determine the sequence of all genes in an individual for this project was approximately $150,000, but that this cost will likely decrease considerably in the future.
More information: Science Magazine: www.sciencemag.org
Source: Johns Hopkins Medical Institutions