Mutation leading to kidney disease in Cypriot families is traced back to one ancestor more than 300 years ago
A study published Online First in The Lancet has identified a genetic mutation in the immune system which leads to chronic kidney disease in those affected. Furthermore, all the families affected so far are of Cypriot origin and the researchers believe this mutation represents a significant proportion of the kidney disease burden in Cyprus and in Cypriot families worldwide -- and that the mutation dates back to a single common ancestor at least 16 generations ago.
The Article is by Professor Patrick Maxwell, The Rayne Institute, University College London, UK, and colleagues, and is funded by the UK Medical Research Council and The Wellcome Trust.
In the Article, the researchers have identified the disease—which they have named CFHR5 nephropathy—in 28 people from five families. All are of Cypriot descent and some are living in the UK. Symptoms include blood in the urine—sometimes microscopic, sometimes visible—and progressive kidney malfunction.
Existing guidelines state that, if not accompanied by traces of protein, urinary tract abnormalities or impairment to the kidneys, blood in the urine is considered benign. But the researchers show in this new study that in certain cases it can signal progressive chronic kidney disease.
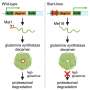
The researchers, based in the UK, Cyprus, France, and Spain, identified an inherited kidney disorder caused by the mutation in gene CFHR5. Many mutations are caused by changing single letters in the genetic code, but here the change is a duplication of quite a large chunk of DNA consisting of several thousand letters. CFHR5 produces one of the proteins of the complement system, a key part of the body's built-in immune response.
Another interesting finding was that the risk of progressive kidney disease is more common in men than women. Researchers say that people of either sex who carry just one copy of the variation will almost certainly show some signs of kidney injury, but in women it may more frequently be a little blood in the urine which will be picked up on a dipstick test. The chance of a child inheriting the condition where one of their parents is affected is 50%. The researchers have developed a simple DNA test which would mean that an embryo could be tested to see whether it has the faulty gene, as can happen for Huntington's Disease and other genetic conditions. In such cases, in-vitro fertilisation (IVF) is carried out and the embryo is screened before being implanted into the mother. Genetic counseling can be offered to individuals with or at risk of the variation, including family planning. The researchers have also used the genetic test in kidney donation from family members. Prof Maxwell says: "Obviously one would not want to take a kidney from someone with the CFHR5 mutation and give it to a brother/sister/child/parent who also has the disease."
The authors say that their genetic analysis suggests the mutation probably dates back 16 generations (more than three centuries) to a single ancestor. They say: "High penetrance of blood in the urine, the wide geographical distribution of ancestry within Cyprus, and the presence of affected individuals in the UK suggests that this disease will account for a substantial proportion of renal disease affecting inhabitants of the island and their descendants worldwide."
The authors predict that this one mutation could be responsible for between 1 and 2% of all kidney disease cases in Cypriots. Further analysis that does not form part of this study suggests that a minimum of about 1 person in every 6,000 Cypriots has the mutation.
In addition, the authors discuss the implications of their work on the immune system beyond the scope of the paper. Complement is a key aspect of the innate immune system and the authors say that with CFHR5 one of the 'brakes' on complement activation is working less well. The complement system is particularly important in combating childhood infections, before antibodies have developed. As a result of removing one of these brakes, the complement response to an infection might be more pronounced, and perhaps more effective. So, children having the CFHR5 mutation may in fact be more resistant to childhood infections, despite their poor kidney disease prognosis.
In a linked Comment, Dr S Ananth Karumanchi, Beth Israel Deaconess Medical Center and Harvard Medical School, Boston, MA, USA and Dr Ravi Thadhani, Massachusetts General Hospital and Harvard Medical School, Boston, MA , USA, say that treating physicians will ask what can be done for these patients in addition to standard treatments for chronic kidney disease.
They say: "Maxwell and colleagues have provided a first step towards development of targeted therapies, and as such, the future for CFHR5 nephropathy and related conditions is positive. If abnormal CFHR5 protein is mainly made in the liver, we can explore whether liver transplantation offered before onset of severe renal disease leads to cure. We might also be able to show whether treatment with eculizumab or other complement-targeted drugs would be efficacious."
More information: www.thelancet.com