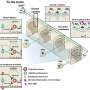
New undertsanding of gut hormones and gut function sheds light on obesity
Research on obesity examining the role of hormones and the autonomic functions of the digestive system was presented at the 75th Annual Scientific Meeting of the American CoIlege of Gastroenterology.
Gastric function, as well the activities of the autonomic nervous system that regulates digestion, are impaired in obese individuals in both fasting and fed states, according to a study from the University of Texas Medical Branch in Galveston, "Altered Postprandial Gastric and Autonomic Functions in Obese Subjects." Measures of gastric myoelectrical activity (GMA) by electrogastrography and of heart rate variability on electrocardiogram for 12 obese and 12 lean patients were compared for a 30 minute fasting period and then 30 minutes after a fatty soup or a high protein soup.
"Obese subjects in the study showed enhanced responses to both soups," said the study's co‐author Jiande Chen, Ph.D. "The obese were more receptive to fatty meals, meaning the stomach is more tolerant to fatty meals, as well as more responsive to protein meals. Since the function of the stomach is to pump whatever is in the stomach to the small intestine, being more responsive means that the stomach may empty the protein meals more quickly in obese subjects than in lean subjects," explained Dr. Chen.
Researchers observed that the percentage of normal slow waves was reduced with the fatty soup in the lean group, but not in the obese. The power of gastric slow waves was not altered with the protein soup in the lean, but increased in the obese.
According to Dr. Chen, "Obese patients are more prone to fatty meals. The stomach of lean subjects gets 'sick' (a reduction in normal slow waves of the stomach) with fatty soup, whereas the stomach of obese subjects is fine with fatty soup. The increase in the power of gastric slow waves with the protein soup in obese, but not in lean, suggests that the stomach responds to protein soup more positively and the emptying of the stomach may be faster in obese than in lean."
Additionally, researchers found reduced activity for the vagus nerve that regulates muscle contraction of the stomach and intestines to help process food among obese subjects in the study, and increased activity in the sympathetic nervous system in the fasting state.
The obese demonstrated a complete absence of normal autonomic responses after eating. "Typically, after a meal in lean subjects, the cardiac sympathetic activity increases and the cardiac vagal activity decreases," said Dr. Chen. "In the obese subjects, however, these normal post‐meal changes in the cardiac autonomic functions were completely absent, which suggests an impaired autonomic response to food ingestion. The autonomic nervous system sends meal‐related gastrointestinal information, such as mechanical distention and chemical stimulation via nutrients to the brain. If the response of the autonomic system to food ingestion is impaired or altered, the brain may not be fully informed of the food ingestion, which may lead to over‐eating," explained Dr. Chen.
Gut Hormone Obestatin Predicts Weight Loss after Bariatric Surgery
Investigators from Inova Health System led by Zobair Younossi, M.D., FACG, assessed the relationship between weight loss after bariatric surgery and circulating hormones, "Baseline Serum Obestatin Correlates with Rate of Weight Loss After Bariatric Surgery." Among 35 patients undergoing Roux‐en‐Y gastric bypass surgery, the rate of weight loss was correlated with only one circulating hormone, obestatin, a peptide produced in the gut which may have a role in appetite suppression.
"We know there is an inverse relationship between obestatin and body mass index," explains James Michael Estep, Ph.D., the lead author of the study. In this study, weight loss among patients after bariatric surgery was faster during the first three months and even for the first 24 months, and a high baseline obestatin level measured just prior to surgery was strongly associated with the rate of weight loss after surgery.
Obestatin is thought to suppress appetite; there is experimental evidence from model organisms that obestatin is involved in the regulation of appetite, metabolism, and inflammation in a complex and somewhat antagonistic relationship with ghrelin (with which obestatin shares the same genetic locus.) However, the mechanism of its activity, down to the receptor with which it binds, remains unknown.
"Our promising results indicate that obestatin is certainly worth pursuing in a larger cohort study as an indicator of the efficacy of bariatric surgery, especially within the first year," concluded Dr. Estep.