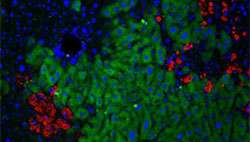
Immunofluorescent staining of liver two months after normal liver cells (green) were transplanted into a transgenic mouse model of alpha-1 antitrypsin disease. Red indicates the mutated protein that has accumulated in the host liver cells, and clusters of blue cells (concentrated in upper left) are the transplanted cells that have markedly proliferated.
Transplanting cells from healthy adult livers may work in treating a genetic liver-lung disorder that affects millions of people worldwide, according to an animal study in the April 18 online edition of the Journal of Clinical Investigation. Jayanta Roy-Chowdhury, M.D., professor of medicine and of genetics at Albert Einstein College of Medicine of Yeshiva University, is the study’s senior author.
The genetic disorder, alpha-1 antitrypsin (AAT) deficiency, is the most common potentially lethal hereditary disease among Caucasians, affecting an estimated 100,000 people in the United States and 3.4 million people worldwide. AAT is a protein made by the liver that is essential for lung health. In AAT deficiency, the liver produces a misshapen form of AAT that cannot enter the bloodstream and instead gets stuck inside liver cells, causing two major problems:
• AAT accumulates in the liver, leading to fibrosis (development of scar tissue) and liver failure;
• Too little AAT reaches the lungs, where it’s needed to rein in elastase, an enzyme produced by white blood cells. Elastase helps kill bacteria in the lungs, but uncontrolled elastase activity can damage lung tissue and lead to severe emphysema (chronic obstructive pulmonary disease).
In the study, Dr. Roy-Chowdhury and his colleagues tested cell therapy on transgenic mice whose liver cells (hepatocytes) had been engineered to produce mutant human AAT, resulting in liver fibrosis. When the mice were given infusions of hepatocytes harvested from the livers of healthy mice, the transplanted cells proliferated in the host liver, progressively replacing diseased hepatocytes. Most importantly, said Dr. Roy-Chowdhury, the transplanted cells reversed the fibrosis that had developed.
Current therapy for AAT deficiency consists of life-long injections of a genetically engineered version of AAT called Prolastin. “This very expensive therapy slows progression of the lung disease in some patients but does not have any beneficial effect on the liver disease,” said Dr. Roy-Chowdhury. The only other therapy for AAT deficiency is combined lung-liver transplantation, which is reserved for the sickest patients.
“These promising results in animals indicate that it may be worthwhile to investigate the usefulness of hepatocyte transplantation for AAT deficiency as well as a variety of other inherited liver-based disorders,” said Dr. Roy-Chowdhury.
The title of the paper is “Spontaneous hepatic repopulation in transgenic mice expressing mutant human alpha 1-anti-trypsin by wildtype donor hepatocytes.” Other Einstein researchers involved in the study are Jianqiang Ding, M.D., Ph.D., Namita Roy-Chowdhury, Ph.D., Yesim Avsar, M.D., and Chandan Guha, M.B., B.S., Ph.D. The research was supported by the National Institutes of Health, the National Institute of Diabetes, Digestive and Kidney Diseases, the New York Stem Cell Foundation, the Oxalosis and Hyperoxaluria Foundation, and the United States Department of Defense.
Provided by Albert Einstein College of Medicine