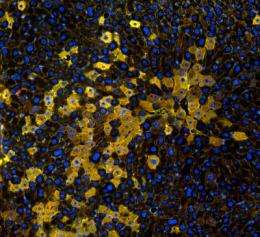
These are regenerative liver cells eight weeks after transplantation. Credit: Yoon-Young Jang
Johns Hopkins researchers have demonstrated that human liver cells derived from adult cells coaxed into an embryonic state can engraft and begin regenerating liver tissue in mice with chronic liver damage.
The work, published in the May 11 issue of the journal Science Translational Medicine, suggests that liver cells derived from so-called "induced-pluripotent stem cells (iPSCs)" could one day be used as an alternative to liver transplant in patients with serious liver diseases, bypassing long waiting lists for organs and concerns about immune system rejection of donated tissue.
"Our findings provide a foundation for producing functional liver cells for patients who suffer liver diseases and are in need of transplantation," says Yoon-Young Jang, M.D., Ph.D., assistant professor of oncology at the Johns Hopkins Kimmel Cancer Center. "iPSC-derived liver cells not only can be generated in large amounts, but also can be tailored to each patient, preventing immune-rejection problems associated with liver transplants from unmatched donors or embryonic stem cells."
iPSCs are made from adult cells that have been genetically reprogrammed to revert to an embryonic stem cell-like state, with the ability to transform into different cell types. Human iPSCs can be generated from various tissues, including skin, blood and liver cells.
Although the liver can regenerate in the body, end-stage liver failure caused by diseases like cirrhosis and cancers eventually destroy the liver's regenerative ability, Jang says. Currently, the only option for those patients is to receive a liver organ or liver cell transplant, a supply problem given the severe shortage of donor liver tissue for transplantation. In addition, mature liver cells and adult liver stem cells are difficult to isolate or grow in the laboratory, she says. By contrast, iPSCs can be made from a tiny amount of many kinds of tissue; and the embryonic stem-like iPSCs can grow in laboratory cultures indefinitely.
For the study, Jang and colleagues generated human iPSCs from a variety of adult human cells, including liver cells, fibroblasts (connective tissue cells), bone marrow stem cells and skin cells. They found that though the iPSCs overall were molecularly similar to each other and to embryonic stem cells, they retained a distinct molecular "signature" inherited from the cell of origin.
Next, they chemically induced the iPSCs to differentiate first into immature and then more mature liver cell types. Regardless of their origin, the different iPSC lines all showed the same ability to develop into liver cells.
Using mice with humanlike liver cirrhosis, the researchers then injected the animals with either 2 million human iPSC-derived liver cells or with normal human liver cells. They discovered that the iPSC-derived liver cells engrafted to the mouse liver with an efficiency of eight to 15 percent, a rate similar to the engraftment rate for adult human liver cells at 11 percent.
Researchers also found the engrafted iPSCs worked well. The scientists detected proteins normally secreted by adult human liver cells, including albumin, alpha-1-antitrypsin, transferrin and fibrinogen, in the blood of mice transplanted with human iPSC-derived liver cells.
Additional studies will need to be completed before clinical trials can begin, Jang says. One concern has been the potential for embryonic stem cells or iPSCs to cause tumors, though no tumors formed in any of the transplanted mice during the seven months they were studied (equating to more than 30 years in a human life). The scientists also plan to evaluate the impact of molecular memory that may linger in iPSCs for other type of cellular fate changes.
Provided by Johns Hopkins Medical Institutions