Artificial thymus tissue enables maturation of immune cells
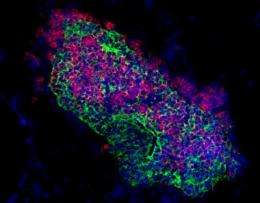
The thymus plays a key role in the body's immune response. It is here where the T lymphocytes or T cells, a major type of immune defence cells, mature. Different types of T cells, designated to perform specific tasks, arise from progenitor cells that migrate to the thymus from the bone marrow. Researchers at the Max Planck Institute of Immunology and Epigenetics in Freiburg have generated artificial thymus tissue in a mouse embryo to enable the maturation of immune cells. In this process, they discovered which signalling molecules control the maturation of T cells. Their results represent the first step towards the production of artificial thymus glands that could be used to replace or augment the damaged organ.
As part of the immune response, the T cells are responsible for tracking down and destroying intruders and degenerated cells in the body. Their progenitors are formed in the bone marrow. Attracted by chemical signals, they migrate from there to the thymus. This small organ, which is located above the heart, is divided into niches that provide the cells with environmental conditions necessary for their different development phases. The cells mature there into different types of T cells, which are eventually released into the body.
Signalling substances that are active in the various niches of the thymus play a crucial role in the maturation of the progenitor cells. A combination of four proteins – the two chemokines Ccl25 and Cxcl12, and the cytokine Scf and the Notch ligand DLL4 – determines whether progenitor cells are attracted to a particular niche in the thymus and how they develop there. It was not previously known which combination of factors is responsible for the development of a particular cell type.
Researchers from the Max Planck Institute in Freiburg have now succeeded in explaining the control mechanism. "The development of the progenitor cells depends on surprisingly few factors and follows simple rules," says Thomas Boehm. "For example, just two factors, namely Cxcl12 and DLL4, are sufficient for the T cell progenitors to complete half of their development. From that point, it takes just a few steps until two types of mature T cells with the CD4 and CD8 surface molecules are formed. Previously, it was assumed that the control process was far more complicated," explains the scientist.
In order to test how the different combinations of the four genetic factors affect the maturation and differentiation of the immune cells, the researchers created an artificial thymus environment in the mouse embryo. To do this, they switched off the transcription factor Foxn1. Fox1 ensures that all of the genes in the DNA that code for the four different proteins are read. Foxn1 is thus a kind of "general switch" with which all of the relevant genes can be turned off all at once. Having generated non-functional thymus tissue in this way, the researchers then activated the genes again individually and in combination and observed the associated effects on the development of the progenitor cells.
Interestingly, the scientists were also able to attract the progenitors of B lymphocytes and of mast cells to the artificial thymus environment and allow them to mature there. These two types of immune cells normally only develop in the bone marrow. By switching off the Notch ligand DLL4, the researchers were also able to control the maturation of these cells in the artificial thymus. This would suggest that the genetic factors at work in the bone marrow are similar to those in the thymus.
"Our results are not only of relevance to the understanding of fundamental immunological processes," says Thomas Boehm. "They also constitute early milestones in the development of artificial thymuses. This means that one day we may be able to help patients whose thymus has been damaged, for example as a result of cancer treatment," hopes the scientist.
More information: Lesly Calderón, Thomas Boehm, Synergistic, context-dependent and hierarchical functions of epithelial components in thymic microenvironments, Cell, 30 March 2012.