Lung cancer is the most lethal cancer in the United States. According to the National Cancer Institute, lung cancer causes more than 150,000 deaths annually and has a survival rate of 16 percent. More Americans die of lung cancer each year than of cervical, breast, colon and prostate cancers combined.
Currently, cancer screening -- checking people for cancers or pre-cancers before symptoms appear -- is widely supported for breast (mammography), colorectal (colonoscopy and other techniques) and cervical (Pap smears) cancers. While regular screening for these cancers is standard practice, lung cancer screening is not.
Now, results of a large, randomized, controlled trial conducted by Rush University Medical Center scientist Dr. James L. Mulshine, and co-researchers showed that screening with low-dose spiral computed tomography (CT) not only reduces lung cancer deaths but would cost insurers less than colorectal, breast and cervical cancer screenings.
Mulshine is vice president and associate provost at Rush University Medical Center. The study was published in the April 2012 issue of the journal Health Affairs.
"The core of our cost-benefit calculation was a stage-shift model, in which an intervention — in this case, lung cancer screening — shifted the distribution of stages of cancer," the researchers wrote. "The consequence of the stage shift was that more lung cancers were detected at an earlier stage. This leads to treatment costs that are earlier and lower, and to more people cured of or living with cancer, both changes that are quantified by our calculation."
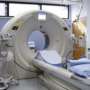
Low-dose spiral CT is a rapidly evolving, commonly available, advanced imaging technology in which x-ray detectors rotate around the body to produce a three-dimensional image of internal structures. Today, a full low-dose spiral CT lung cancer screening can be completed in a few seconds.
Several studies of asymptomatic people at high risk for lung cancer showed that low-dose spiral CT can detect early-stage disease. A national study of 54,000 people ages 55 to 74 at high risk for lung cancer demonstrated that use of three annual screens with low-dose spiral CT was associated with a 20 percent reduction in cancer-related death, compared with surgical removal of the tumor alone.
In people younger than 65, lung cancer accounts for 43,000 deaths per year, which is about 26 percent of the annual number of all lung cancer deaths. Lung cancer incidence roughly doubles with each five-year age band from 45 to 49 to 60 to 64 years. It then increases more slowly until 75 to 79 years, after which it begins declining.
The current study model was designed to estimate the cost and cost-benefit of lung cancer screening for high-risk US smokers and former smokers ages 50 to 64, each of whom had smoked one or more packs of cigarettes a day for at least 30 years. The group had private commercial medical insurance (that is, they were not covered by Medicare, Medicaid or another form of public insurance.) This group comprises about 18 million people, or about 30 percent of the US population ages 50 to 64.
Results of this study suggest that commercial insurers should consider lung cancer screening of high-risk individuals to be high-value coverage and provide it as a benefit to people who smoked at least one pack a day for 30 or more years.
The authors also believe that payers and patients should demand screening from high-quality, low-cost providers thus helping set an example of efficient system innovation.
"Our study suggests opportunities for the efficient implementation of lung cancer screening, which would involve insurers; selection of high-quality providers; and use of "best published practices" for managing clinical aspects of screening, along with rigorous tracking of outcomes. The goal would be to ensure achievable standards for quality and cost," the researchers said.
Mulshine's colleagues on this study were Bruce S. Pyenson, Marcia Sander, Yiding Jiang and Howard Kahn. They are actuaries with the consulting firm Milliman, in New York.
Provided by Rush University Medical Center