New guidelines issued for biopsy use in melanoma patients
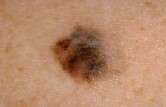
(HealthDay) -- Sentinel lymph node biopsy -- a minimally invasive surgical technique that lets doctors see whether cancer has spread -- should be performed on patients with melanoma tumors of intermediate thickness and may also be appropriate for thick melanoma tumors, according to new guidelines released Monday.
The American Society of Clinical Oncology (ASCO) and the Society for Surgical Oncology issued the evidence-based recommendations to clarify the use of this type of biopsy, which they said has been inconsistent.
A sentinel lymph node is the first lymph node to which cancer cells are most likely to spread from the original tumor, according to the U.S. National Cancer Institute. There can be more than one sentinel lymph node. During a biopsy, the node is identified, removed and examined for cancer cells.
"When used for the right patients at the right time, sentinel lymph node biopsy is one of our best tools for personalizing melanoma treatment, and for sparing patients from unnecessary procedures or therapies," study lead author Dr. Sandra Wong, co-chair of the guideline panel and an assistant professor of surgery at the University of Michigan, said in an ASCO news release.
The panel of 14 clinical and methodological experts from various disciplines reviewed 73 studies, involving 25,000 patients, that were published over the past two decades. After examining this evidence, the panel made the following recommendations:
- The procedure is recommended for all patients with melanoma tumors between 1 millimeter (mm) and 4 mm (intermediate thickness). Sentinel lymph node biopsy detects cancer in the sentinel node in about 18 percent to 26 percent of these patients, the panel noted.
- Sentinel lymph node biopsy may be beneficial to patients with melanoma tumors greater than 4 mm ("thick"). The panel noted, however, that few studies focus on the use of the biopsy in patients with thick melanomas.
- The panel found there is not enough evidence to recommend routine sentinel lymph node biopsy for patients with melanoma tumors less than 1 mm ("thin"). The experts added that thin melanomas can usually be cured through surgical removal of the primary tumor. However, the biopsy could be considered in patients with thin melanoma who have certain high-risk factors, such as rapidly dividing cancer cells.
Patients with a positive sentinel lymph node biopsy should undergo complete removal of the remaining lymph nodes, the experts added. This procedure has been shown to prevent the spread of cancer.
The panel also advised doctors to discuss sentinel lymph node biopsy, particularly the procedure's potential risks and benefits, with their patients as part of the treatment-planning process.
"Our rapidly growing understanding of the biology of melanoma is driving development of more effective treatments with fewer side effects for patients," panel co-chair Dr. Gary Lyman, a professor of medicine and director of comparative effectiveness and outcomes research at Duke University School of Medicine and the Duke Cancer Institute, said in the news release.
"But to take advantage of this progress, we need to know the true extent of the disease from the start. This guideline will help ensure that sentinel lymph node biopsy is used appropriately whenever it can provide that vital information while avoiding unnecessary procedures in patients who are unlikely to benefit."
Information on the guidelines was published online by ASCO.
More information:
The U.S. National Cancer Institute has more about melanoma.
Copyright © 2012 HealthDay. All rights reserved.














