UCSF team engineers 'safety switches' for immune therapies

(Medical Xpress) -- A UCSF team has harnessed a natural protein in bacteria to create a “pause switch” in immune cells, potentially leading to more effective and safer immune therapies for diseases such as cancer and multiple sclerosis.
These “effector proteins” are produced by some bacteria to protect themselves from their host’s immune system and work by infiltrating immune cells and shutting down the immune response long enough to allow the bacteria to replicate.
In new findings published online July 22 in the journal Nature, the team of cellular engineers showed that they could remove those effector proteins from bacteria and engineer them into yeast or human immune T cells to create a “pause switch” in the engineered cell.
Ultimately, they hope to program that pause switch into immune therapies to make them easier to control and thus less prone to side effects.
Immune therapies are a growing interest in several fields, particularly cancer and autoimmune diseases, such as multiple sclerosis and diabetes. The goal of these therapies is to either bolster the immune system to kill diseased cells, such as cancer cells, or calm down an overactive immune response, as occurs in autoimmune diseases. Immune therapies are showing increasing promise in the clinic, but those therapies can be difficult to control in the body and can end up killing healthy host cells as well as their targets, researchers said.
“There’s a lot of excitement now about harnessing the immune system to combat cancer and autoimmune diseases,” said senior author Wendell Lim, PhD, a Howard Hughes Medical Investigator and professor of Cellular and Molecular Pharmacology at UCSF. “It’s been well established that we can retrain the immune system to attack disease cells, but you have to do it in a controlled way. It’s like learning to ski — the first thing you have to learn is how to stop.”
Normally, when researchers engineer T cells for therapeutic use, the only way to stop those cells from being overactive is to insert DNA encoding a “self-destruct” switch, which destroys the cells. This new approach tells the cells to pause, rather than die.
Lim, who oversees the UCSF Cell Propulsion Lab, focuses his cellular engineering research on creating a cellular tool kit – the brakes, gas and steering wheel — for scientists to insert into biological therapies to control them better, just as we hone chemistry-based drugs to make them more precise and less toxic.
Bacteria, it turns out, are a good source of those tools, with a range of activities that enable them to survive in the hostile environment of the host’s gut or mouth.
“The immune system is always a question of balance. If we can decide when and where these therapies will turn on, the precision will be much higher,” Lim said. “There are a lot of very powerful proteins that pathogens have evolved that we can harness to do that.”
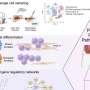
The new findings demonstrated that two bacterial effector proteins — Yersinia pestis effector YopH and the Shigella flexneri OspF protein — could be used to rewire and fine-tune a critical chain of proteins in a cell known as the mitogen-activated protein (MAP) Kinase pathway, which plays an important role in immune responses and in regulating the uncontrolled cell growth associated with cancer.
The authors also showed that the OspF protein could be selectively aimed at one of several MAPK pathways in the same cell, and that this activity can only be restored through new protein synthesis, which slows the immune response even further.
The co-first authors on the paper are Ping Wei and Wilson W. Wong (now at Boston University), both postdoctoral fellows in Lim’s lab in the Department of Cellular & Molecular Pharmacology, and in the Howard Hughes Medical Institute. Co-authors include Jason S. Park, and Sergio G. Peisajovich (now at University of Toronto), also with the department and HHMI; and Ethan Corcoran (now at Northwest Permanente NC) and Arthur Weiss, with HHMI and the UCSF Department of Medicine. The team is also part of the UCSF Cell Propulsion Laboratory and the UCSF Center for Systems and Synthetic Biology.
The research was funded by fellowships from the American Cancer Society, the Li Foundation and the California Institute for Regenerative Medicine, as well as through support from the National Institutes of Health, the National Science Foundation Synthetic Biology and Engineering Research Center, the Packard Foundation and the Howard Hughes Medical Institute.
More information: The abstract is available online.