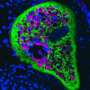
Host genome controls skin microbiota and inflammation
Numerous recent studies linked gut microbiota with various diseases such as obesity or diabetes. Little is known, however, on how gut and skin microbiota composition is controlled. In a recent study published in the journal Nature Communications on 17 September, John Baines, Saleh Ibrahim and their colleagues of the Inflammation Research Excellence Cluster show that composition of skin microbiota is controlled by the host genome and that skin bacteria may have a greater influence on inflammatory diseases than previously thought. Their landmark findings will open the door to identify gene variants controlling skin microbiota and to define their link to various diseases such as skin inflammatory disorders.
The human body contains more bacteria than human cells. Most of these bacteria comprise the normal gut and skin microbiota. Susceptibility to chronic inflammatory diseases is determined by immunogenetic and environmental risk factors that include resident microbial communities. Whether these differences are of primary etiological importance or secondary to the altered inflammatory environment remains largely unknown.
The inflammation cluster research groups led by Saleh Ibrahim of the University of Lübeck, and John Baines of the MPI and CAU, correlated the genomic variations of hundreds of mice that partially develop skin inflammatory diseases with skin microbiota. They showed evidence for host gene-microbiota interactions contributing to disease risk in a mouse model of autoantibody-induced inflammatory skin disease. Furthermore they identified genetic loci contributing to skin microbiota variability, susceptibility to skin inflammation and their overlap. The majority of the identified microbiotal communities are characterized by reduced abundance being associated with increased disease risk, providing evidence of a primary role in protection from disease.
These findings offer a promising potential for using those probiotic species for preventative and therapeutic treatment development. John Baines: "It appears that the skin flora is a phenotype that is partially controlled by the host genome variations. This in turn predisposes to the development of disease. The more we learn about these interactions, the more possibilities there will be for a better and more individualized treatment and prevention of skin inflammatory diseases.
More information: Genome-wide mapping of gene-microbiota interactions in susceptibility to autoimmune skin blistering. DOI: 10.1038/ncomms3462