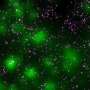
Insulin secretion disrupted by increased fatty acids
Patients with type 2 diabetes have increased levels of circulating glucose and fatty acids, which lead to disease complications. In healthy individuals, β cells within pancreatic islets release insulin in response to glucose and incretins, which are gastrointestinal hormones. Coordination between β cells is predicted to be important for insulin release.
In this issue of the Journal of Clinical Investigation, David Hodson and colleagues at Imperial College London demonstrate that ? cell-? cell interactions are important for insulin secretion in human islets and that these interactions are regulated by incretins. The authors found that increased fatty acid levels suppressed incretin-associated insulin release.
These findings indicate that therapies aimed at maintaining ? cell connectivity may be useful for restoring glucose balance in type 2 diabetes.
More information: Lipotoxicity disrupts incretin-regulated human ? cell connectivity, J Clin Invest. DOI: 10.1172/JCI68459
Abstract
Pancreatic ? cell dysfunction is pathognomonic of type 2 diabetes mellitus (T2DM) and is driven by environmental and genetic factors. ? cell responses to glucose and to incretins such as glucagon-like peptide-1 (GLP-1) and glucose-dependent insulinotropic polypeptide (GIP) are altered in the disease state. While rodent ? cells act as a coordinated syncytium to drive insulin release, this property is unexplored in human islets. In situ imaging approaches were therefore used to monitor in real time the islet dynamics underlying hormone release. We found that GLP-1 and GIP recruit a highly coordinated subnetwork of ? cells that are targeted by lipotoxicity to suppress insulin secretion. Donor BMI was negatively correlated with subpopulation responses to GLP-1, suggesting that this action of incretin contributes to functional ? cell mass in vivo. Conversely, exposure of mice to a high-fat diet unveiled a role for incretin in maintaining coordinated islet activity, supporting the existence of species-specific strategies to maintain normoglycemia. These findings demonstrate that ? cell connectedness is an inherent property of human islets that is likely to influence incretin-potentiated insulin secretion and may be perturbed by diabetogenic insults to disrupt glucose homeostasis in humans.