Heart attack gene, MRP-14, triggers blood clot formation
Right now, options are limited for preventing heart attacks. However, the day may come when treatments target the heart attack gene, myeloid related protein-14 (MRP-14, also known as S100A9) and defang its ability to produce heart attack-inducing blood clots, a process referred to as thrombosis.
Scientists at Case Western Reserve School of Medicine and University Hospitals Case Medical Center have reached a groundbreaking milestone toward this goal. They have studied humans and mice and discovered how MRP-14 generates dangerous clots that could trigger heart attack or stroke, and what happens by manipulating MRP-14. This study describes a previously unrecognized platelet-dependent pathway of thrombosis. The results of this research will appear in the April edition of the Journal for Clinical Investigation (JCI).
"This is exciting because we have now closed the loop of our original finding that MRP-14 is a heart attack gene," said Daniel I. Simon, MD, the Herman K. Hellerstein Professor of Cardiovascular Research and Medicine at the School of Medicine and director of the University Hospitals Harrington Heart & Vascular Institute. "We now describe a whole new pathway that shows clotting platelets have MRP-14 inside them, that platelets secrete MRP-14 and that MRP-14 binds to a platelet receptor called CD36 to activate platelets."
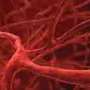
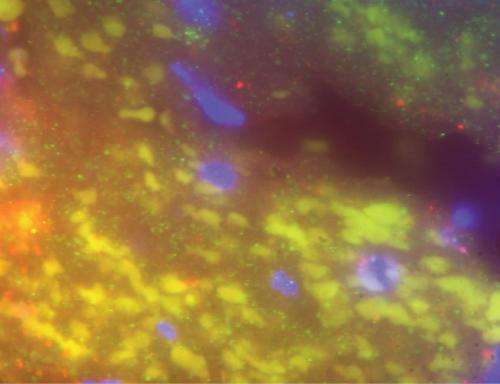
This translational research has moved back and forth from the cardiac catheterization laboratory investigating patients presenting with heart attack to the basic research lab probing mechanisms of disease. The clinical portion of this research yielded a visually stunning element—blood clots extracted from an occluded heart artery loaded with MRP-14 containing platelets.
"It is remarkable that this abundant platelet protein promoting thrombosis could have gone undetected until now," Simon said.
In detailed studies using MRP-14-deficient mice, the investigators discovered MRP-14 in action. One key finding is that, while MRP-14 is required for pathologic blood clotting, it does not appear to be involved in the natural, primary hemostasis response to prevent bleeding.
"The practical significance of this research is that it may provide a new target to develop more effective and safer anti-thrombotic agents," Simon said. Current anti-clotting drugs are subject to significant bleeding risk, which is associated with increased mortality.
"If we could develop an agent that affects pathologic clotting and not hemostasis, that would be a home run," Simon said. "You would have a safer medication to treat pathologic clotting in heart attack and stroke."