New techniques for the prevention and treatment of chronic sores
The latest Empa "Technology Briefing" took place at the end of April in St Gallen, dealing with the the treatment and prevention of chronic sores. Specialists from healthcare sector, science and the med-tech industry used the event to network and update on recent developments. A number of experts active in various branches of the field gave presentations on their most recent work.
As the average age in our society continues to increase, more and more people are suffering from chronic sores. In an ideal world this would be preventable, or at least the wounds could be treated so as to heal well without leaving scars. However current methods of treatment have only been partially successful and therefore there is great interest in new therapeutic techniques.
Juerg Traber, Director of the Bellevue Vein Clinic in Kreuzlingen, began the day by presenting an overview of chronic sores and their treatment. Amongst the topics he dealt with was the difficulty of defining what exactly is a "chronic" sore. Guidelines do exist, but every patient has their own individual set of conditions and sores are of different sizes – factors which influence the rate of healing. "You wouldn't expect a large area sore to heal completely in six weeks, but this doesn't necessarily mean that you're dealing with a case of chronic sores," he maintained. Normally a sore should heal in 4 to 6 weeks, and if this does not happen it may be an indication of chronic status. Exactly how these kinds of chronic wounds are treated in the course of day-to-day operations was described by the Head of Nursing at the Bellevue Vein Clinic, Maria Signer, with the help of examples drawn from real-life.
A range of approaches to prevention
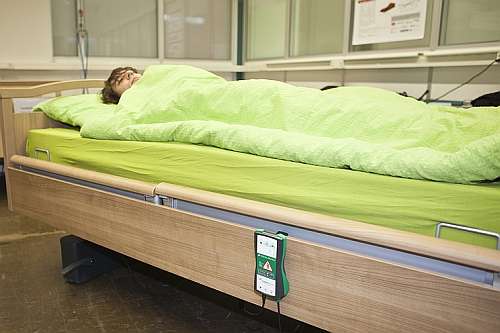
Several companies have developed products aimed at preventing sores from becoming chronic in the first place. Compliant Concept, a spin-off of Empa and the ETH Zurich, has for example developed its "Mobility Monitor", a sensor which records the movements of patients as they are sleeping. Sickness or treatment with pain relieving medication can lead to a situation where patients do not move regularly when asleep.

This frequently causes bedsores, known in medical terms as decubitus ulcers, where the tissue around the pressure point dies, creating an open wound. The Mobility Monitor provides information to the healthcare staff on when and how often a patient should be turned in order to prevent bedsores from forming. Observation of 11 test patients over a two-week period showed that without the use of the Mobility Monitor, nursing staff tended to move their bedridden charges more often than was necessary. Using the Mobility Monitor allowed carers to reduce the rate of patient movement by around 40%, which not only reduced the work load on the medical staff but also meant that patients were disturbed less frequently during sleep.
A new bed sheet for use by bedridden patients, developed and tested by Empa and the Schoeller company, was presented by Anke Scheel-Sailer, Medical Director of the Research and Rehabilitation Quality Management Department at the Swiss Paraplegic Centre, Nottwil.
The surface of the bed sheet is microstructured which reduces the contact area, and therefore friction, on the skin when compared to conventional bedcovers. A study conducted by the Paraplegic Centre has shown that the novel bed sheets are indeed effective in preventing bedsores.
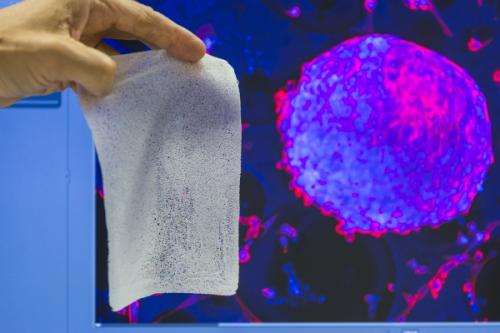
Absorbable dressings and plant-based healing agents
There have also been advances in the treatment of chronic bedsores. In collaboration with the Nolax company, Empa has further developed a special "wound foam", an absorbable biocompatible polymer which encourages the closure and healing of chronic sores. Conventional dressings must be regularly changed, disturbing and possibly delaying the healing process. The new material offers a novel dressing which gradually becomes populated with connective tissue cells, while the polymer component simultaneously decomposes. The new skin layer is all that remains behind, as Katja Nuss of the University of Zürich's Competence Centre for Applied Biotechnology and Molecule Medicine reported. The material has also already been tested on animals.
Empa researcher Arie Bruinink of the "Materials-Biology Interactions Laboratory" and his team have optimised the material and structure of the wound dressing so that it is non-toxic, becomes populated with human cells and – depending on its particular composition – dissolves away in one or two weeks.
Using an elaborate process, a three-dimensional cell structure consisting of around 15,000 human cells was created to test whether cells would actually populate the dressing. Generally speaking Bruinink and his colleagues use such cell and tissue cultures to develop functional and biocompatible materials for use within the human body. "Our aim is to develop in vitro methods which have a high prognostic value when applied to in vivo situations," said Bruinink.