Highly drug resistant, virulent strain of Pseudomonas aeruginosa arises in Ohio
A team of clinician researchers has discovered a highly virulent, multidrug resistant form of the pathogen, Pseudomonas aeruginosa, in patient samples in Ohio. Their investigation suggests that the particular genetic element involved, which is still rare in the United States, has been spreading heretofore unnoticed, and that surveillance is urgently needed. The research is published ahead of print in Antimicrobial Agents and Chemotherapy.
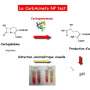
The P. aeruginosa contained a gene for a drug resistant enzyme called a metallo beta-lactamase. Beta-lactamases enable broad-spectrum resistance to beta-lactam antibiotics, including carbapenems, cephalosporins, and penicillins, because they can break the four atom beta-lactam ring, a critical component of these antibiotics' structure.
The initial isolate of metallo-beta-lactamase-producing P. aeruginosa was identified in March, 2012, in a foot wound of a 69-year-old man with type 2 diabetes living in a long-term care facility. During 2012-2013, the investigators identified this highly antibiotic-resistant infection in six other patients. One of the seven patients subsequently died of the infection.
The cases are linked epidemiologically via admission to a community hospital and residence in long-term care facilities in Northeast Ohio. The one exception was a patient from Qatar who was transferred into a tertiary medical center in Ohio, says lead author Federico Perez, of the Louis Stokes Cleveland Department of Veterans Affairs Medical Center, Cleveland, Ohio, USA.
The investigators subsequently found that the metallo beta-lactamase was contained within an integron, a genetic element that can jump from one species of bacterium to another, can reside on plasmids or within the chromosomes, and is known for being able to contain multiple antibiotic resistance genes.
This particular metallo beta-lactamase, verona integron-encoded metallo beta-lactamse (VIM), is widespread globally, if not in the US. "VIM enzymes confer resistance to imipenem and all other beta-lactams," says Perez. "They are not inhibited by metallo beta-lactamase inhibitors."
"Alarmingly, the [extensively drug-resistant] phenotype expressed by some of these isolates precluded any reliable antibiotic treatment since they even displayed intermediate resistance to colistin, an 'agent of last resort'," the researchers write. "Patients who were affected had multiple comorbidities, endured prolonged colonization, required long-term care and, in one instance had a lethal outcome from a bloodstream infection."
On top of everything else, genomic sequencing and assembly showed that the integron was part of a novel 35 kilobase region that included a transposon (another mobile genetic element) and the so-called Salmonella Genomic Island 2 (SGI2). That indicated that a recombination event had occurred between Salmonella and P. aeruginosa, contributing even more resistance genes to the latter.
"This is the first description of genetic exchange of a large mobile element—the Salmonella Genome Island—and resistance genes between P. aerugenosa and Salmonella, says Perez. "This movement of genetic material creates concern that metallo beta-lactamases will disseminate rapidly in these enteric pathogens that are also very invasive. We are also concerned about the possibility of enhanced virulence."
More information: The manuscript can be found online at aac.asm.org/content/early/2014 … 372-14.full.pdf+html . The final version of the article is scheduled for the October 2014 issue of Antimicrobial Agents and Chemotherapy.










.jpg)