NIH announces winners of 2014 Undergraduate Biomedical Engineering Competition

Four winning teams were announced in the Design by Biomedical Undergraduate Teams (DEBUT) challenge, a biomedical engineering design competition for teams of undergraduate students. The judging was based on four criteria: the significance of the problem being addressed; the impact on clinical care; the innovation of the design; and the existence of a working prototype. The first place team will receive $20,000, second $15,000 and the two teams that tied for third will both receive $10,000 in a ceremony at the annual Biomedical Engineering Society (BMES) conference in October. The challenge was managed by the National Institute of Biomedical Imaging and Bioengineering (NIBIB), which is a part of the National Institutes of Health.
The first place winning project, AccuSpine, addresses the problem of postoperative neurological or vascular complications that result from the more than 20 percent of screws placed incorrectly along the spine during the nearly 500,000 spinal fusion surgeries performed each year in the United States. The undergraduate team of seven students from Johns Hopkins University, Baltimore, designed an improved pedicle probe, a device used to create a path for the screws, aimed at reducing breaches in spinal fusion procedures. The AccuSpine provides feedback to the surgeon through vibrations and LED lights, warning them when a breach is detected.
Second place was awarded to the Sensory Substitution Glove project by a team of three seniors from Boston University. The glove was created to supplement the traditional white cane used by those with visual impairments. While the cane can help warn people of immediate impediments, it cannot sense obstacles at head-height or give much warning of sudden drop-offs, giving its users very little time to react. Ultrasound and infrared sensors, an accelerometer, a microprocessor, and a small speaker attached to the back of the glove scan the surroundings to provide vibrational signals that give the user a broader understanding of the world around him without limiting the use of the hand. By simply making different gestures, the user can adapt the sensor area, creating a wider or narrower sensing angle depending on the needs of the moment.

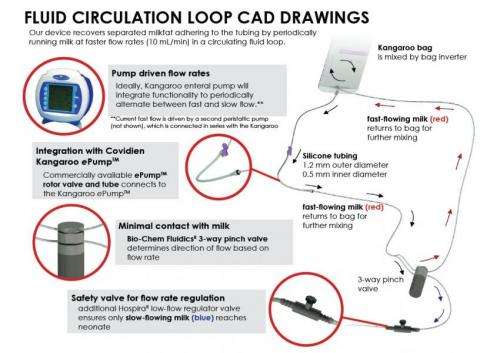
Third place prize was shared by two innovative projects. The first, Nutriflow, created by a team from Rice University, Houston, addresses a problem associated with tube feeding of mother's breast milk in infants who are of low birth weight. In current feeding systems, up to 50 percent of the fat content in breast milk can separate from the aqueous portion of milk, adhering to the bag and tube and never reaching the infant. Since the fat contains essential nutrients and calories, this can slow weight gain and cause other adverse health effects. The Nutriflow device is a low cost solution that flips the feed bag at regular intervals which keeps the fat from separating out of the milk. In addition, every five minutes the milk in the tube is diverted from the infant back to the bag for further mixing, reducing the amount of time milk is stagnant. The system has been shown to increase the fat content that reaches the infant from about 58 percent up to 95 percent.
The second, A Diaper Based System for Neonatal Urine Collection, Dehydration Assessment and Bacterial Infection Detection, was designed by a team from the University of California, Riverside, to provide an early warning of illness from dehydration or bacterial infection in countries where current technologies are not available. The system is inexpensive and does not require electricity or a clinic to confirm the results. A simple diaper liner changes color to confirm low pH (dehydration) as well as leukocytes, nitrites, and other chemical changes that indicate severe problems, providing a low cost, point-of-care diagnosis.
"We are very proud to announce the winning projects," said NIBIB Director Roderic I. Pettigrew, Ph.D., M.D. "All four of them show how a fresh perspective can create inexpensive, effective, and transformative technologies to solve longstanding challenges in healthcare. I am excited to see how this next generation of biomedical engineers will continue to create technology that is better, faster, and less costly."
There were 63 eligible entries received from 33 universities in 19 different states.



















