Sun damage and cancer

Around 30 Australians are diagnosed with melanoma every day and more than 1,200 die from the disease each year.
While small amounts of ultraviolet (UV) radiation are required for the production of vitamin D to keep bones and muscles strong and healthy, skin can burn from just 15 minutes of exposure to the summer sun.
In 2009, the World Health Organization (WHO) classified the whole ultraviolet spectrum and the use of solariums as carcinogenic to humans, placing them in the same category as asbestos and tobacco. The majority of skin cancers in Australia are thought to be caused by exposure to UV radiation in sunlight.
The sun emits three different types of UV radiation: UVA, UVB and UVC. While UVC rays are filtered by the ozone, 10% of UVB and 95% of UVA rays reach the earth's surface.
Cell damage
The UV effects on the skin are largely dependent on the type of UV rays (proportion of UVB and UVA), the amount and intensity of UV, and the stage at which the cells on the skin are in during their normal division and renewal process.
UV can produce a number of effects within the cell including specific types of DNA damage in skin cells and, with extreme UV exposure, cell death. Some of these types of oxidative DNA and nucleotide damage, and failure of the cells to repair this damage can prompt cells to mutate, leading to the development of skin cancers.
With some cancers that develop on skin exposed to excessive sunlight, DNA damage can be identified through UV-specific DNA mutations within the tumour.
But sun exposure that doesn't result in burning may still damage the skin cells. Research suggests that regular exposure to UV radiation year after year can also lead to skin cancer.
Repairing DNA
When cells are actively dividing and proliferating they are particularly vulnerable to DNA damage. So cells are equipped with mechanisms to respond to and repair DNA damage within the cell to restore the DNA structure before they continue dividing.
The cells respond by delaying progression through the cell cycle through the cooperation of cell cycle checkpoints and several biochemical pathways. This allows sufficient time for repair before the critical phases of the cell division process proceed.
In the event the DNA damage is too severe, the cells kill themselves off, preventing DNA damage being transferred to the daughter cells.
If these checkpoints are defective and do not delay the cell cycle progression to enable repair, the result may be an increase in DNA mutations and chromosomal defects. This can cause uncontrolled growth, transformation of the cell and the development of cancer.

In the rare hereditary disease xeroderma pigmentosum (XP), which is caused by defects in some of the normal DNA repair genes, patients display approximately 3000-fold increases in the rate of skin cancer. This emphasises how critical the DNA response and repair process is to UV induced DNA damage.
Skin cancer growth
The top layer of skin, the epidermis, contains three different kinds of cells:
- squamous cells that make up the top outer layer of the skin
- basal cells that make up the lower layer and produce new skin cells as old ones die off
- melanocytes are the bottom layer of the epidermis that produce pigment called melanin, which gives the skin its colour.
Cancer begins when normal cells change and grow uncontrollably. The tumour can be benign (non-cancerous) or malignant (cancerous, and can spread to other parts of the body).
The three major types of skin cancer – melanoma, squamous cell carcinoma (SCC) and basal cell carcinoma (BCC) – are defined by the cell type of the skin from where they develop.
Melanoma
Melanocytes cluster together in the skin during childhood to form moles, and are the cells that produce melanin to help protect the skin from UV radiation.
Melanoma develops in melanocytes, and is the most dangerous and aggressive form of skin cancer, accounting for 3% of all skin cancers. Melanomas can grow very quickly if left untreated and can spread to other parts of the body.
Melanoma of the skin can appear as a new or existing spot, freckle or mole that changes in colour, size or shape and can have dark coloured pigment or no colour in the lesion. They can grow anywhere on the body, not just in areas exposed to the sun.
Non-melanoma skin cancers

Non-melanoma skin cancers are the most common cancers in Australia, and refer to all the types of cancer that occur in the skin that are not melanoma. The two main types are squamous cell carcinomas (SCC) and basal cell carcinomas (BCC), in addition to other rarer forms.
Approximately 28% of skin cancers are SCCs, arising from the squamous cells of the epidermis. This type of skin cancer is mainly caused by UV radiation either from sun exposure or solariums, but it can appear on skin that has been burned, damaged by chemicals, or exposed to x-rays.
About 68% of skin cancers are BCCs, arising in the basal cells in the epidermis. BCCs are mainly caused by long-term exposure to UV radiation from the sun or can develop in people who received radiation therapy as children. This type of skin cancer usually grows slowly.
Protecting against UV damage
A number of environmental factors influence the amount of UV radiation we are exposed to throughout the day, including the earth's latitude, height of the sun throughout the day, cloud cover and reflection of surfaces.
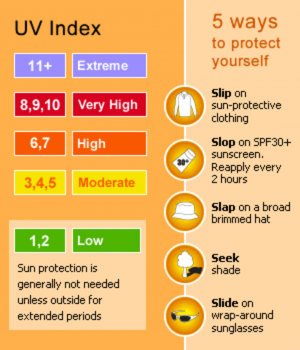
Most Australians need sun protection when the UV index is three or above. UV radiation levels in northern states are higher than southern states, so in some parts of Australia, sun protection is needed all year around at certain times of the day.

To reduce your exposure to UV, cover up when outdoors and use a high-sun protection factor, water-resistant sunscreen that blocks both UVA and UVB rays, and reapply every two hours.
In Australia, we need to balance the risk of skin cancer from too much sun exposure with maintaining adequate vitamin D levels. During summer, most people can maintain adequate vitamin D levels from a few minutes of exposure to sunlight on their face, arms and hands or the equivalent area of skin in the morning or late afternoon when the UV index is below three.
You can check the UV index in the weather section of daily newspapers, on the Bureau of Meteorology website or by using the SunSmart app.
This story is published courtesy of The Conversation (under Creative Commons-Attribution/No derivatives).
![]()

















