Molecular link between obesity and type 2 diabetes reveals potential therapy
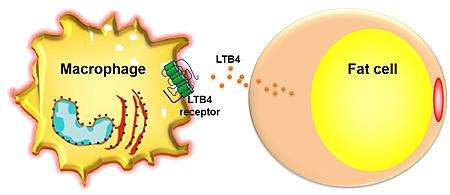
Obesity causes inflammation, which can in turn lead to type 2 diabetes. What isn't well established is how inflammation causes diabetes—or what we can do to stop it. Researchers at University of California, San Diego School of Medicine have discovered that the inflammatory molecule LTB4 promotes insulin resistance, a first step in developing type 2 diabetes. What's more, the team found that genetically removing the cell receptor that responds to LTB4, or blocking it with a drug, improves insulin sensitivity in obese mice. The study is published Feb. 23 by Nature Medicine.
"This study is important because it reveals a root cause of type 2 diabetes," said Jerrold M. Olefsky, MD, professor of medicine, associate dean for scientific affairs and senior author of the study. "And now that we understand that LTB4 is the inflammatory factor causing insulin resistance, we can inhibit it to break the link between obesity and diabetes."
Here's what's happening in obesity, according to Olefsky's study. Extra fat, particularly in the liver, activates resident macrophages, the immune cells living there. These macrophages then do what they're supposed to do when activated—release LTB4 and other immune signaling molecules to call up an influx of new macrophages. Then, in a positive feedback loop, the newly arriving macrophages also get activated and release even more LTB4 in the liver.
This inflammatory response would be a good thing if the body was fighting off an infection. But when inflammation is chronic, as is the case in obesity, all of this extra LTB4 starts activating other cells, too. Like macrophages, nearby liver, fat and muscle cells also have LTB4 receptors on their cell surfaces and are activated when LTB4 binds them. Now, in obesity, those cells become inflamed as well, rendering them resistant to insulin.
Once Olefsky and his team had established this mechanism in their obese mouse models, they looked for ways to inhibit it. First, they genetically engineered mice that lack the LBT4 receptor. When that approach dramatically improved the metabolic health of obese mice, they also tried blocking the receptor with a small molecule inhibitor. This particular compound was at one time being tested in clinical trials, but was dropped when it didn't prove all that effective in treating its intended ailment. Olefsky's team fed the prototype drug to their mice and found that it worked just as well as genetic deletion at preventing—and reversing—insulin resistance.
"When we disrupted the LTB4-induced inflammation cycle either through genetics or a drug, it had a beautiful effect—we saw improved metabolism and insulin sensitivity in our mice," Olefsky said. "Even though they were still obese, they were in much better shape."