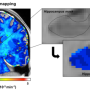
Low sugar uptake in brain appears to exacerbate Alzheimer's disease
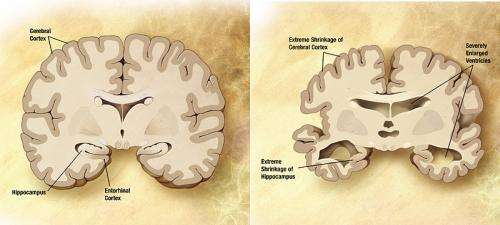
A deficiency in the protein responsible for moving glucose across the brain's protective blood-brain barrier appears to intensify the neurodegenerative effects of Alzheimer's disease, according to a new mouse study from the Keck School of Medicine of the University of Southern California (USC).
The research suggests that targeting the protein called GLUT1 could help prevent or slow the effects of Alzheimer's, especially among those at risk for the disease. The study, "GLUT1 reductions exacerbate Alzheimer's disease vasculo-neuronal dysfunction and degeneration," appears in today's online edition of the peer-reviewed scientific journal Nature Neuroscience.
"Our results suggest that GLUT1 deficiencies at the blood-brain barrier are not just symptoms of Alzheimer's but, in fact, lead to a series of vascular injuries that worsen the effects of the disease," said Berislav V. Zlokovic, M.D., Ph.D., director of the Zilkha Neurogenetic Institute (ZNI) at the Keck School of Medicine, the Mary Hayley and Selim Zilkha Chair for Alzheimer's Disease Research and the study's principal investigator. "We do not know yet whether medicine can restore GLUT1 expression, but we believe that targeting the protein may help prevent Alzheimer's from getting worse among individuals predisposed to develop the disease."
According to the Alzheimer's Association, roughly 5.2 million people of all ages in the United States today have Alzheimer's disease, an irreversible, progressive brain disease that causes problems with memory, thinking and behavior. It is the most common type of dementia, a general term for loss of memory and other mental abilities, and is projected to affect 16 million Americans over age 65 by 2050.
Glucose is the brain's main energy source, and GLUT1 helps move it across the blood-brain barrier, a cellular layer that prevents entry of blood and pathogens into the brain. Previous research has shown diminished glucose uptake in the brain among individuals at genetic risk for Alzheimer's disease, with a positive family history, and/or who develop the disease but show mild or no cognitive impairment.
In this new study, Zlokovic's team used transgenic mice to show that GLUT1 is necessary to maintain proper brain capillary networks, blood flow and blood-brain barrier integrity. They found that GLUT1 deficiency led to diminished glucose uptake into the brain as early as two weeks of age and, by six months of age, neuronal dysfunction, behavioral deficits, elevated levels of amyloid-beta peptide, behavioral changes and neurodegenerative changes. The team also found that GLUT1 deficiency in the endothelium - the inner lining of blood vessels - initiated breakdown of the blood-brain barrier. Alzheimer's disease pathogenesis is widely believed to be driven by amyloid-beta peptide build-up in the brain, facilitated by breakdown of the blood-brain barrier.
Areas of future research may include identification of the metabolic pathways through which GLUT1 deficiencies in the blood-brain barrier influence brain metabolism as well as an examination of whether early embryonic GLUT1 loss affects the central nervous system differently than a deficiency incurred later during development.
More information: Winkler, E. A., Nishida, Y., Sagare, A. P., Rege, S. V., Bell, R. D., Perlmutter, D. ... Zlokovic, B. V. (2015). GLUT1 reductions exacerbate Alzheimer's disease vasculo-neuronal dysfunction and degeneration. Nature Neuroscience, 1-10. Published online March 2, 2015; DOI: 10.1038/nn.3966