Central sleep apnoea device increases mortality in heart failure
Adaptive servo-ventilation (ASV) therapy increases mortality and should not be used to treat central sleep apnoea in heart failure patients with reduced ejection fraction, the SERVE-HF trial shows.
The Hot Line study, presented at ESC Congress 2015, and published simultaneously in the New England Journal of Medicine, "provides practice-changing guidance for the treatment of chronic heart failure (CHF)," said Martin Cowie, MD, co-principal investigator of the study, from Imperial College London, in London, UK.
"This study has changed our understanding of sleep-disordered breathing in systolic heart failure – the text books will have to be rewritten," he commented. "Doctors now know that treatment of central sleep-disordered breathing by mask therapy is not helpful for these patients and might be harmful. Lives will be saved by the findings of this new study."
Professor Cowie emphasized that patients in the study had reduced ejection fraction and predominantly central sleep apnoea, and therefore the results cannot be generalized to patients with preserved ejection fraction or obstructive sleep apnoea.
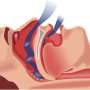
Unlike obstructive sleep apnoea, central sleep apnoea (CSA) is caused by the brain failing to trigger breathing during sleep.
ASV is designed to detect significant variation in breathing and deliver pressure through a face mask in order to maintain a normal breathing pattern.
In SERVE-HF (which stands for The Treatment of Sleep-Disordered Breathing With Predominant Central Sleep Apnoea by Adaptive Servo Ventilation in Patients With Heart Failure) 1,325 chronic heart failure patients with a reduced ejection fraction who were randomised to receive either guideline-based medical management alone (control group), or with the addition ASV for a recommended 5 hours per night, 7 days a week.
After a median follow-up of 31 months ASV effectively treated central sleep apnoea but had no effect on the primary end point, which was a combination of all-cause death, life-saving cardiovascular intervention, or unplanned hospitalisation for worsening heart failure.
The event rate for the primary outcome was 54.1% in the ASV group compared to 50.8% in the control group (hazard ratio [HR] 1.13; P=0.10).
Moreover, the addition of ASV to standard care had no beneficial effect on functional measures, including quality-of-life, six-minute walk distance, or symptoms.
However, all-cause mortality and cardiovascular mortality were higher in the ASV group than in the control group (34.8% versus 29.3%; HR 1.28; P=0.01 and 29.9% versus 24.0%; HR 1.34; P=0.006).
"The early and sustained increase in cardiovascular mortality seen with ASV was unexpected, and the reasons for this effect remain unclear," said Professor Cowie, noting that the SERVE-HF results are contrary to findings from some previous studies.
One possible explanation for this is that central sleep apnoea may actually be a compensatory mechanism in some heart failure patients, he suggested.
"Potentially beneficial consequences of central sleep apnoea in these patients could be that it rests respiratory muscles, and modulates excessive sympathetic nervous system activity, and by diminishing this effect ASV may be detrimental for patients with heart failure."
Although SERVE-HF did not meet its primary endpoint, "it was a well-designed and executed study," concluded Professor Cowie, "and because of it we now know that ASV therapy is contraindicated in this subset of chronic heart failure patients."