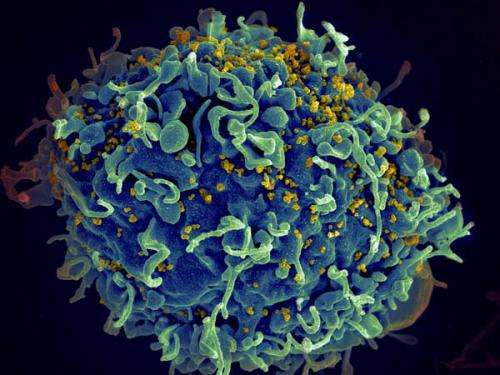
HIV, the AIDS virus (yellow), infecting a human immune cell. Credit: Seth Pincus, Elizabeth Fischer and Austin Athman, National Institute of Allergy and Infectious Diseases, National Institutes of Health.
The District of Columbia's needle exchange program prevented 120 new cases of HIV infection and saved an estimated $44 million over just a two-year period, according to a first-of-a-kind study published today by researchers at the Milken Institute School of Public Health (Milken Institute SPH) at the George Washington University.
"Our study adds to the evidence that needle exchange programs not only work but are cost-effective investments in the battle against HIV," says Monica S. Ruiz, PhD, MPH, an assistant research professor in the Department of Prevention and Community Health at Milken Institute SPH. "We saw a 70 percent drop in newly diagnosed HIV cases in just two years. At the same time, this program saved the District millions of dollars that would have been spent for treatment had those 120 persons been infected."
The new study, published in the scientific journal, AIDS and Behavior, may help to inform the ongoing debate among policymakers about whether to provide funding for programs that distribute sterile injection equipment to drug users. Last spring, health officials in Indiana's Scott County created a needle exchange program to deal with injection drug use and the rapid spread of HIV—and local officials in other parts of the U.S. are considering the same move. Critics argue that such programs encourage illicit drug use. But other research has shown that drug users who come in for clean needles often get other health services-including referral to programs that treat drug addiction.
In 1998, Congress banned the use of federal funds for needle exchange programs but did allow states and cities to use locally generated revenues to establish such exchanges—and many cities did just that. However, the ban continued to affect the District of Columbia, making it the only city in the nation which could not use municipal funds to start such a program. Finally, in December 2007, legislation was passed that lifted the so-called DC ban and the city's Department of Health moved swiftly to start a program that included needle exchange and referrals to HIV testing and addiction treatment programs.
Ruiz and her colleagues examined how this change in policy affected the HIV epidemic in terms of actual new cases associated with injection drug use. The research team used surveillance data to determine the actual number of new injection drug use (IDU)-related cases of HIV following the removal of the DC ban and the implementation of the needle exchange network. Next, the team used a modeling technique to forecast how many cases of HIV would have occurred had the DC ban remained in place.
They found that, if the DC ban had remained in place, an estimated 296 injection drug users would have gotten HIV during the two-year study period. In fact, once the ban was removed and the District launched its needle exchange network, only 176 new cases of IDU-associated HIV occurred. "The lifting of the DC ban prevented about 120 injection drug users from becoming infected in just two years," Ruiz says. "Furthermore, the DC needle exchange program continues to reduce the number of new cases of HIV among injection drug users in the city."
Needle exchange programs help the most disadvantaged and vulnerable people, including drug users and people who exchange sex for drugs, says Ruiz, adding that the program is a potent weapon in the war against AIDS. Despite recent progress against HIV, the District of Columbia still has one of the worst epidemics of HIV in the nation, according to the U.S. Centers for Disease Control and Prevention.
Past research has looked at how well needle exchange programs work: For example, a Washington state study found that a needle exchange program led to more than an 80 percent reduction in the new cases of hepatitis B and C infections—both blood-borne diseases that also can be passed on through the use of dirty needles. And a New York program demonstrated that giving drug users clean needles resulted in a 70 percent drop in new HIV infections.
However, the study by Ruiz and colleagues also looked at the cost savings associated with this policy change event in DC. Ruiz and her colleagues took estimates from the U.S. Centers for Disease Control and Prevention on the average lifetime cost of treating HIV and calculated that averting 120 cases of HIV infection would lead to a savings of about $44.3 million.
Many injection drug users are covered by publicly funded health plans. If HIV transmission is prevented, savings would accrue as a result of not having to treat HIV infection over the course of the person's life. "Thus, it could be reasoned that the $44.3 million in savings is money that is saved by taxpayers," Ruiz says.
Such needle exchange programs are relatively inexpensive to operate. For example, the District allocated just $650,000 per year for the first 24 months of the program and it provides more than just access to clean needles. Drug users can also get an HIV test, free condoms—which also prevent sexually transmitted diseases—and it is often the only connection that drug users have to a regular source of health care, including tests that can spot an emerging problem like hepatitis.
More information: Ruiz and her colleagues published the study, "Impact Evaluation of a Policy Intervention for HIV Prevention in Washington, DC," online in the journal AIDS and Behavior.
Journal information: AIDS and Behavior
Provided by George Washington University