A potential role for fat tissue as an HIV reservoir and source of chronic inflammation
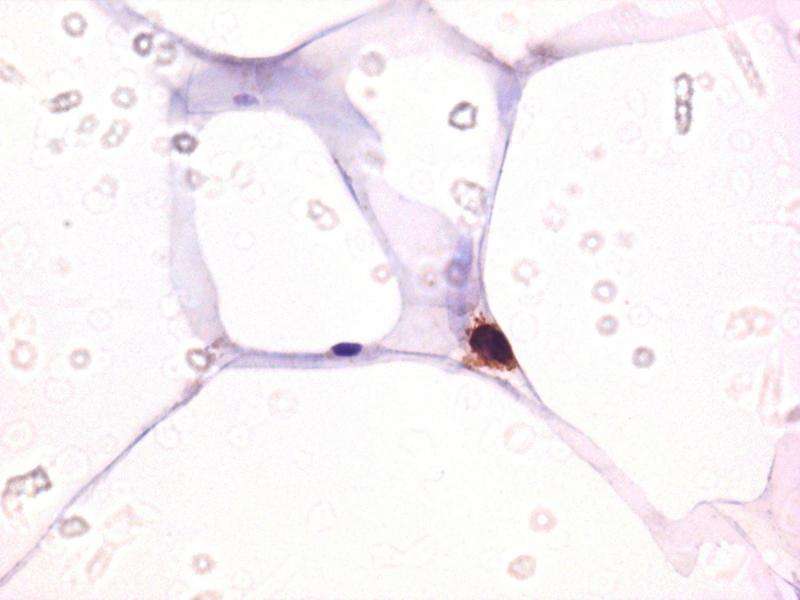
Viral persistence and chronic inflammation are two key features of HIV-positive patients on antiretroviral therapy (ART). A study published on September 24th in PLOS Pathogens reports results from macaques and humans that suggest an important role for adipose (fat) tissue as an HIV reservoir with inflammatory potential.
The establishment and persistence of low-grade inflammation in HIV-positive individuals on ART are not well understood. Given that adipose tissue (which makes up between 15 and 20% of the body weight in healthy people) is a source of inflammation in obese individuals, Christine Bourgeois and Olivier Lambotte, from the University Paris SUD, France, and colleagues, decided to investigate a possible role of the adipose tissue in humans infected with HIV and in macaques infected with simian immunodeficiency virus (SIV, an HIV relative that causes AIDS-like disease in some non-human primates).
They found that SIV infection in macaques is associated with changes in the composition of the adipose tissue: Fat tissue from infected animals has higher densities of both adipocytes (fat storage cells) and a mix of differentiated and undifferentiated cells called stromal vascular fraction or SVF that contains a large proportion of immune cells.
Moreover, these immune cells (CD4+ T cells, CD8+ T cells, and macrophages) show enhanced immune activation and/or inflammatory profiles compared with non-infected animals. The researchers were also able to detect SIV DNA and RNA in the combined total SVF as well as in isolated adipose tissue macrophages and CD4+ T cells.
They observed similar results in ART-controlled, HIV-infected patients who had undergone elective abdominal surgery: their SVF samples are positive for HIV DNA, and the researchers could show the presence of infected and virus-producing cells within the patients' adipose tissue and more specifically among adipose CD4+ T cells.
The researchers conclude that they "identified adipose tissue as a crucial cofactor in both viral persistence and chronic immune activation/inflammation during HIV infection", and propose that "modulating adipose tissue may constitute a valuable means of limiting both viral persistence and chronic inflammation in ART-receiving HIV-infected patients".
More information: Damouche A, Lazure T, Avettand-Fènoël V, Huot N, Dejucq-Rainsford N, Satie A-P, et al. (2015) Adipose Tissue Is a Neglected Viral Reservoir and an Inflammatory Site during Chronic HIV and SIV Infection. PLoS Pathog 11(9): e1005153. DOI: 10.1371/journal.ppat.1005153